
Trauma Room (Crisis Resource Management – Brindley, Cardinal)
Background: Addressing traumatic injuries is a major component of Emergency Medicine (EM) practice. Providers are asked to quickly evaluate these patients, address major life threats, and make a full inventory of injuries. Having a systematic approach is essential to a rapid assessment that minimizes the chance of missing injuries. This post will outline a step-by-step approach to evaluation.
Pre-Arrival
- All providers should don appropriate personal protective equipment including gowns, gloves, facemasks, and face-shields
- If patients are coming in by Emergency Medical Services (EMS), the pre-hospital team will often call ahead with vital signs and information about mechanism of injury
- Mechanism of injury guides evaluation and raises or lowers probability of certain injuries
- Majority of presentations categorized as blunt versus penetrating trauma
- Specific mechanistic considerations include speed of collisions, damage to vehicles, presence of blood at the scene, and other victims or fatalities
- Use this information to prepare for anticipated interventions
- Field vital signs can be used to anticipate potential injuries and prepare interventions
- Mechanism of injury guides evaluation and raises or lowers probability of certain injuries
- Patients are usually triaged based on mechanism of injury or physiologic criteria
- Specific criteria will trigger activation of a trauma team and route patient to resuscitation area
- Most trauma centers have two tiers of activation (eg. level I and level II)
- Multiple providers often respond, including nurses, EM physicians, and trauma surgeons based on level of activation
Trauma Resuscitation (http://www.lasvegasemr.com/)
Arrival
- Most important first step in major trauma (eg. Level I or II) is completion of EMS hand-off
- Give the pre-hospital team silence in the room to give report before beginning patient assessment
- Immediate life threats (agonal respirations, risk of exsanguination) will require immediate management and are often identified by the pre-hospital team
Primary Survey
- Goal is to find and address immediate life threats
- Typical approach is ABCDE mnemonic, standing for airway, breathing, circulation, disability, and exposure
- Although often taught as dictating priority or order of assessment (eg. airway before circulation), all components should be assessed in parallel
Airway
- Look externally for potential obstructions like facial injuries, blood, or vomit
- Have the patient say their name, listening for any gargling or noisy breathing
- Quickly assess mental status and determine whether they are able to clear secretions and keep their tongue from obstructing the airway
Breathing
- Inspect and palpate chest wall for injury. Look at the position of the trachea and for JVD. Inspect work of breathing
- Visualization of the neck will require temporary removal of the C-collar
- Listen for breath sounds bilaterally
- Assess the patient’s O2 saturation as a marker of oxygenation. Attach EtCO2 or observe respirations to assess ventilation
EFAST in Trauma (Army.mil)
Circulation
- Look for any major sources of external bleeding. Assess for internal bleeding with rapid physical exam
- Often augmented by an Extended Focused Assessment with Sonography in Trauma (E-FAST)
- 5 major locations patients can exsanguinate
- Chest
- Abdomen/pelvis
- Retroperitoneum
- Long bone (eg. femur)
- Street (externally)
- Pediatric patients can bleed out from head injuries due to lower blood volume (scalp lacerations or, rarely, intracranial hemorrhage)
- In blunt trauma, the presence of any vital sign abnormalities may prompt empiric placement of a pelvic binder
- Check the patient’s blood pressure
- Palpate radial and dorsalis pedis pulses bilaterally
- Assess for presence, quality, and rate
- Presence of pulses in particular anatomic locations were previously used as markers of a certain BP, however this has found to be inaccurate (Deakin 2000, Poulton 1988)
Disability
- Examine the pupils
- Calculate the Glasgow coma scale (GCS)
- Look for movement of all extremities
Exposure
- Remove all clothing from the patient
- Re-cover the patient with warm blankets
- Log roll to assess for injuries in the back
Secondary Survey
- Divided into focused AMPLE history and head to toe physical exam
- May be abbreviated in unstable patients as they progress to surgery, imaging, or interventional radiology
AMPLE History
- If patient is unable to provide history, try to obtain information from pre-hosptial team, family members or witnesses
- AMPLE mnemonic is often used
- Allergies
- Medications
- Ask specifically about anticoagulants
- Past medical history
- Last meal
- Events/Environment
- Obtain a clear history of the events leading up to and after the injury
- Ask in general about injuries sustained and specifically about head injures
- If there is concern for a head injury, ask about loss of consciousness and vomiting
Physical Exam
- HEENT
- Examine the scalp for bleeding
- Palpate the scalp, face and jaw for tenderness
- Examine the pupils again for size and reactivity
- Examine the ears for hemotympanum
- Examine the nose for septal hematoma
- Examine the oral cavity for injuries or broken teeth
- Ask the patient to close their mouth and ask if teeth alignment feels normal
- C-Spine
- If your patient is in a C-collar, have an assistant maintain spinal precautions while you remove the collar
- Note that patients with penetrating trauma should not be placed in C-collars due to increased mortality (Oteir 2015)
- Palpate the cervical spinous processes for tenderness
- Midline tenderness is concerning for spine injury and should prompt consideration of cervical spine imaging
- Be specific with location tenderness
- If your patient is in a C-collar, have an assistant maintain spinal precautions while you remove the collar
- Thorax
- Feel the shoulder girdle for instability or fractures
- Check the ribs for tenderness or instability
- Recheck lung sounds and perform a cardiovascular exam
-
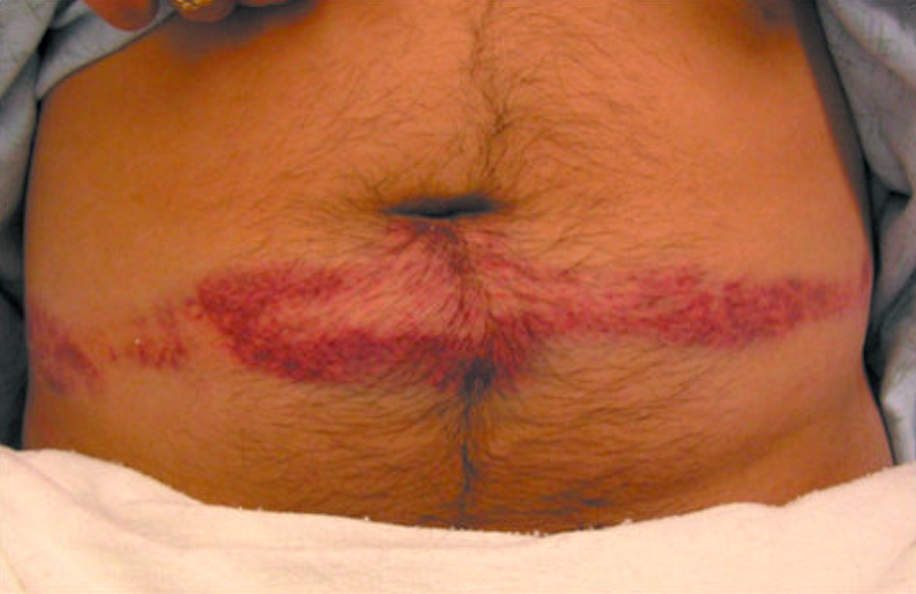
Seat Belt Sign (regionstraumapro.com)
Abdomen/Pelvis
- Examine the abdomen for bruising
- Palpate for tenderness, guarding and rebound
- Avoid rocking pelvis
- If examining for stability, press inward to avoid further injury
- Any suspicion for pelvic injury should dictate placement of a pelvic binder and further manipulation should be minimized (manipulation can lead to worsening of injuries and additional blood loss)
- Extremities
- Check all extremities for strength, sensation, and presence of a pulse
- Range the joints
- Palpate for tenderness and deformity
- Back
- Roll the patient with assistance, maintaining spinal precautions if necessary
- Palpate the spinous processes for tenderness or step-offs
- Digital rectal exam
- Historically included as part of assessment
- Recent literature has questioned the necessity of this practice (Esposito 2005)
- ATLS now recommends DRE as a selective intervention before inserting a urinary catheter (Kortbeek 2008)
- Motor function of L5-S2 can be assessed by asking the patient to flex their gluteal muscles (“squeeze your butt-cheeks”)
Take Home Points
- Development of a systematic approach is essential to rapidly assessing the wide diversity of trauma patients and minimizes missed injures
- Prepare with whatever information is available before the patient arrives and remember to get a good handoff from the pre-hospital team
- Complete the primary survey (ABCDEs) and address immediate life threats
- Obtain a good medical history and remember to complete a comprehensive head-to-toe exam
Read More
EM Basic: Trauma Resuscitation Part 1
REBEL EM: Is ATLS wrong about palpable blood pressure estimates?
Life in the Fast Lane: Digital rectal exam (DRE) in trauma
Taming the SRU: Application of Pelvic Binders
Core EM: How to apply a Pelvic Binder
References
Deakin CD, Low JL. Accuracy of the advanced trauma life support guidelines for predicting systolic blood pressure using carotid, femoral, and radial pulses: observational study. BMJ. 2000;321(7262):673-4. PMID: 10987771
Poulton TJ. ATLS paradigm fails. Ann Emerg Med. 1988;17(1):107. PMID: 3337405
Oteir AO, et al. Should suspected cervical spinal cord injury be immobilised?: a systematic review. Injury. 2015;46(4):528-35. PMID: 25624270
Esposito TJ, et al. Reasons to omit digital rectal exam in trauma patients: no fingers, no rectum, no useful additional information. J Trauma. 2005;59(6):1314-9. PMID: 16394903
Kortbeek JB, et al. Advanced trauma life support, 8th edition, the evidence for change. J Trauma. 2008 Jun;64(6):1638-50. PMID: 18545134
