Definition
Adrenal crisis is a life-threatening emergency due to an acute deficiency of adrenocortical hormones, namely cortisol and aldosterone, which can be fatal if not diagnosed early and treated aggressively. Classically it presents as severe hypotension refractory to IV fluids and vasopressors.
Background
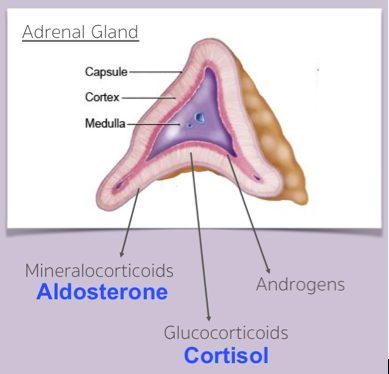
Adrenal glands produce mineralocorticoids (aldosterone), glucocorticoids (cortisol) and androgens in the outer cortex. Catecholamines are produced in inner medullary zone. Classified as primary or secondary in etiology, but both types can lead to adrenal crisis.
Clinical Presentation
- Variable and non-specific complaints – weakness, confusion, fever, nausea, vomiting, abdominal pain
- Shock and fever can be only signs
- Common precipitants – surgery, infection, burn, sepsis, trauma, metabolic or cardiovascular event
- Consider this diagnosis in the following patients:
- Known primary adrenal insufficiency
- Pituitary disease (i.e. secondary adrenal insufficiency)
- Previously or currently on prolonged steroid therapy (especially asthma/COPD)
Primary adrenal insufficiency: disease affecting the adrenal gland
- Addison’s Disease – autoimmune
- Congenital adrenal hyperplasia (CAH) – enzyme deficiency
- Adrenal hemorrhage (Waterhouse-Friedrichsen) – meningococcemia
- Tumors (breast, melanoma)
- Infection (TB, HIV)
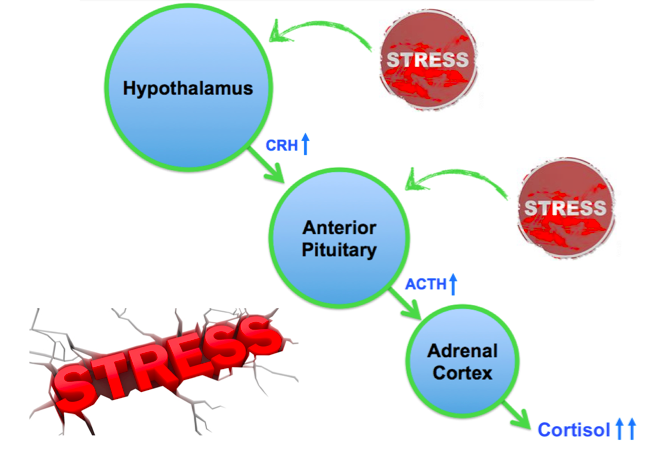
Secondary/Tertiary adrenal insufficiency: ACTH deficiency resulting from pituitary or hypothalamic disease
- Panhypopituitarism
- Pituitary apoplexy – infarction or hemorrhage of tumor
- Chronic steroid therapy (suppresses HPA axis)
- Tumors, granulomas
Diagnostic Studies: CBC, BMP, VBG, fingerstick +/- EKG
- Hypoglycemia
- Hyponatremia (<135mEq/L)
- Hyperkalemia (>5mEq/L)
- Non-anion gap metabolic acidosis
- Low bicarbonate (15-20mEq/L)
- Elevated BUN and creatinine
Management
- Steroid Replacement
- Initial Dose
- Hydrocortisone 100mg
- IV preferred but can be given IM if necessary
- Stress dose hydrocortisone has mineralocorticoid activity (20mg = 0.1mg Florinef)
- Continued dosing: Hydrocortisone 25mg Q6h
- Consider dexamethasone 4mg IV if no known diagnosis of adrenal insufficiency (does not interfere with ACTH stimulation test likely to be performed by inpatient team)
- Even if residual adrenal fx, hydrocortisone dose the same, IVF requirements may just be lower
- Less acute illness may consider 50-100 mg hydrocortisone IM q6h
- Initial Dose
- Hypoglycemia
- Treat severe hyperglycemia with 1-2 gm/kg of D50
- Consider infusion of D5NS for continued hypoglycemia
- Check FS glucose Q1-2 hours to ensure improving hypoglycemia
- Hypotension
- IVF bolus of 30 cc/kg
- Consider using D5NS for resuscitation if the patient has concomitant hypoglycemia
- Blood/urine cultures, antibiotics if infection suspected
- Improvement in BP and clinical picture should occur within 1 hour of 1st dose hydrocortisone
- If Na >130 consider change to D5 ½ NS to avoid rapid rise Na
- If Na <130 and rate of rise slow, continue D5 NS
- Hyperkalemia
- Usually normalized w/ fluids and steroid replacement
- Monitor K Q2-3 hours as may fall during initial rehydration
- See Core EM post on Hyperkalemia for further management
Prevention
- Triple PO steroids if known susceptibility to crisis in setting of physiologic stressors (i.e. influenza, fractures, trauma, surgery, sepsis, myocardial infarction, ischemia, etc.)
- Consider empiric steroids if hx adrenal insufficiency and vomiting/diarrhea, even if otherwise well appearing
- Consider admission in known diagnosis if not able to tolerate PO steroids, needs ongoing parenteral steroids
Take Home Points
- Adrenal insufficiency is a life-threatening emergency; recognize early and treat aggressively
- Hallmark is hypotension refractory to IVF/pressors; < 50% of patients will have a formal diagnosis on presentation
- Suspect in patients with unexplained hypotension and risk factors (prior glucocortocoid use, history of autoimmune disease, hyperpigmentation etc)
- Treat empirically with hydrocortisone 100mg IV and search for precipitating cause
Read More
Sharma AN, Levy DL: Thyroid and Adrenal Disorders, in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2010, (Ch) 128: p 1676-93.
References
Allolio B. Extensive expertise in endocrinology. Adrenal crisis. Eur J Endocrinol. 2015; 172(3): 115-124. PMID: 25288693.
Arlt W, Allolio B. Adrenal insufficiency. Lancet. 2003 May 31;361(9372):1881-93. PMID: 12788587.
Tintinalli JE et al. Adrenal insufficiency and adrenal crisis. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 2011; 7.
Torrey, SP. Recognition and management of adrenal emergencies. Emerg Med Clin North Am. 2005 Aug;23(3):687-702. PMID: 15982541.
Tucci V, Sokari T. The clinical manifestations, diagnosis, and treatment of adrenal emergencies. Emerg Med Clin North Am. 2014; 32(2): 465-484. PMID: 24766944.
Are there no references for this?
Jeff – good question. The information here was from Rosen’s and we’ll update that on the site.