Definition: A serum potassium level > 5.5 mEq/L
Epidemiology
- Common electrolyte disorder
- 10% of hospitalized patients (Elliott 2010)
Causes
- Pseudohyperkalemia: extravascular hemolysis
- Renal failure (potassium is primarily eliminated by the kidneys)
- Acidosis
- Massive cell death (tumor lysis syndrome, rhabdomyolysis, burns, crush injuries, hemolysis)
- Drugs: ACEI, ARBs, Spironalactone, NSAIDs, Succinycholine
Clinical Manifestations
- Mild hyperkalemia often asymptomatic
- Cardiac Effects
- Increased potassium raises the resting membrane potential of cardiac myocytes
- Slows ventricular conduction
- Decreases length of action potential
- Increases cardiac myocyte excitability
- Cardiac effects can manifest in lethal dysrhythmias
- Neuromuscular Effects
- Paresthesias
- Weakness
- Flaccid paralysis
- Depressed or absent deep tendon reflexes
Diagnosis
- Suspect hyperkalemia in ALL patients with renal impairment, especially end-stage renal disease (ESRD)
- Serum potassium
- Can be artificially elevated by extravascular hemolysis
- Blood gas results may differ from standard metabolic panels by up to 0.5mmol/L
- 12-Lead EKG
- Screening test that can rapidly detect severe cardiac manifestations of hyperkalemia
- A normal EKG with a significant serum potassium elevation should raise concerns for spurious results (extravascular hemolysis)
- Sensitivity of EKG to detect hyperkalemia is poor (Wrenn 1991, Aslam 2002, Montague 2008)
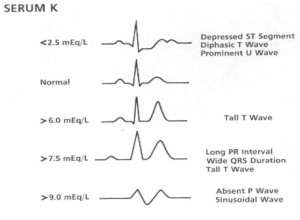
- Classic EKG Findings
- PR prolongation
- Peaked T waves
- Loss of P waves
- Widening of QRS complex
- Sine wave
- Ventricular Fibrillation
- Asystole
- Note: Hyperkalemia can present with a number of “non-classic” EKG findings including AV blocks and sinus bradycardia (Mattu 2000)
- Note: Hyperkalemic EKG changes do not necessarily occur in order (i.e. patients can jump from peaked T waves to sine wave)
Hyperkalemia EKGs
Management
Basics: ABCs, IV, O2, Cardiac Monitor and, 12-lead EKG
- Identify + treat underlying cause of hyperkalemia (i.e. rhabdomyolysis -> hydration)
- Remove inciting factors (i.e. stop ACEI, NSAIDs etc)
Asymptomatic Patients without EKG Changes
- Eliminate potassium from the body
- Sodium Polystyrene (Kayexalate) no proven efficacy
- Enhance renal elimination
- Intravenous hydration if volume depleted
- Consider potassium wasting loop diuretics (i.e. furosemide)
- Dialysis for anuric patients (i.e. ESRD)
Symptomatic Patients or Significant EKG Changes
- Stabilize cardiac myocytes with calcium salts
- Mechanism: Recreates the electrical gradient leading to rapid reversal of cardiac effects and rapid stabilization
- Two Options: CaGluconate, CaCl2
- No difference in time to onset (1st pass metabolism is a myth)
- Dose: 1 ampule CaCl2 (270 mg Ca2+) = 3 ampules CaGluconate (90 mg Ca2+/ampule)
- Onset of action: seconds to minutes
- Duration: 20-30 minutes
- Shift potassium into intracellular space (temporary)
- Insulin
- Mechanism: Activation of the Na-K-ATPase
- Dose: 10 units IV (higher doses quoted but little literature to backup any dose)
- Onset of Action: < 15 min
- Effect: Lowers potassium by about 0.6 mmol
- Duration of action: 30-60 min
- Give with dextrose (0.5 – 1 g/kg) unless hyperglycemia present
- Caution: Duration of action of insulin may outlast administered dextrose. Be vigilant for hypoglycemia
- Beta-adrenoreceptor agonists (i.e. albuterol)
- Mechanism: Activation of beta receptors
- Dose: 10-20 mg inhaled (4-8 standard ampules)
- Onset of Action: < 15 min
- Effect: Lowers potassium by about 0.6 mmol
- Duration of action: 30-60 min
- Additive effect with insulin (Allon 1990)
- Note: Unlikely to have effect in patients taking beta-adrenoreceptor blocker medications
- Sodium Bicarbonate (NaHCO3)
- Evidence for the efficacy of NaHCO3 to lower serum potassium is scant and contradictory (Elliott 2010, Weisberg 2008)
- Eliminate potassium from the body (see above)
- Insulin
Asymptomatic Patients with Minor EKG Changes
- Minimal recommendations on managing this clinical entity
- Eliminate potassium from the body (see above)
- Consider calcium salt administration: patients can rapidly progress through EKG changes and calcium administration may prevent this from occurring. However, the effects of calcium are temporary and offer no long-term protection
- Consider medications to shift potassium intracellularly while waiting for elimination
Take Home Points
- Always obtain an EKG in patients with ESRD upon presentation
- Always obtain an EKG in patients with hyperkalemia as pseudohyperkalemia is the number one cause
- If the patient with hyperkalemia is unstable or has significant EKG changes (wide QRS, sine wave) rapidly administer calcium salts
- In patients who are anuric, early mobilization of dialysis resources is critical
Read More
EMCrit Podcast 32 – Treatment of Severe Hyperkalemia
References
- Elliott MJ et al. Management of patients with acute hyperkalemia. CMAJ 2010; 182(15): 1631-5. PMID: 20855477
- Wrenn K et al. The ability of physicians to predict hyperkalemia from the ECG. Ann Emerg Med 1991; 20(11): 1229-32. PMID: 1952310
- Aslam S et al. Electrocardiography is unreliable in detecting potentially lethal hyperkalaemia in hemodialysis patients. Nephrol Dial Transplant 2002; 17: 1639-42. PMID: 12198216
- Montague BT et al. Retrospective review of the frequency of ECG changes in hyperkalemia. Clin J Am Soc Nephrol 2008; 3:324–330. PMID: 18235147
- Mattu A et al. Electrocardiographic manifestations of hyperkalemia. Am J Emerg Med 2000; 18: 721-9. PMID: 11043630
- Allon M, Copkney C. Albuterol and insulin for treatment of hyperkalemia in hemodialysis patients. Kidney Int 1990; 38:869–872. PMID: 2266671
- Weisberg LS. Management of hyperkalemia. Crit Care Med 2008; 36: 3246-51. PMID: 18936701