Indications for Interscalene Block in the Emergency Department:
- Provides analgesia for clavicle and upper extremity fractures, dislocations, laceration repairs
- Effectively numbs C5-C7 nerve distribution unilaterally, can affect C8-T1 as well but not as reliably
- Most common ED indications include: reduction of shoulder dislocations, proximal humerus fractures, deltoid abscess I & D
- Consider for patients for whom opioids and/or sedation are risky (e.g. elderly, hypotensive)
- May reduce ED length of stay when used as alternative to procedural sedation for glenohumeral joint dislocation reductions
Contraindications:
- Severe coagulopathy
- Local infection near the site of injection
- Respiratory compromise (complications of interscalene nerve block include hemiparesis of the ipsilateral hemidiaphragm due to proximity of the phrenic nerve)
Anatomy:
- The aim of this procedure is to block the brachial plexus trunks in the interscalene groove between the anterior and middle scalene muscles.
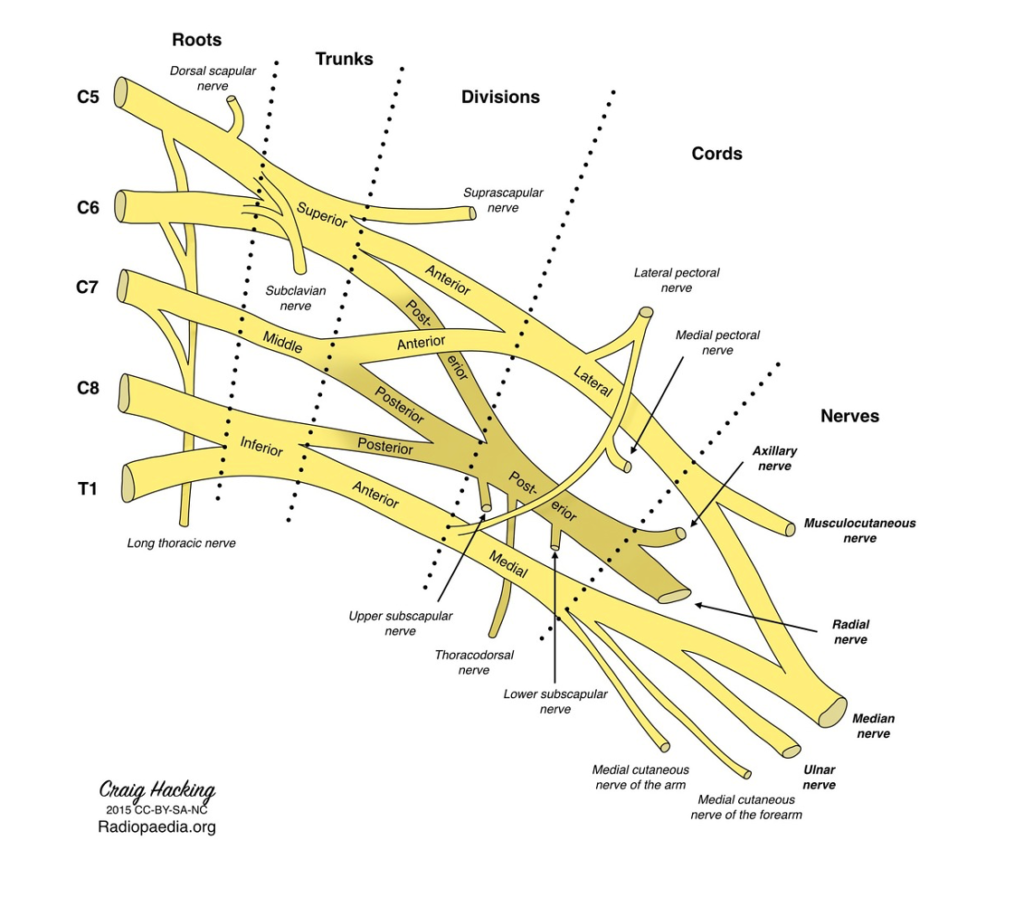
-
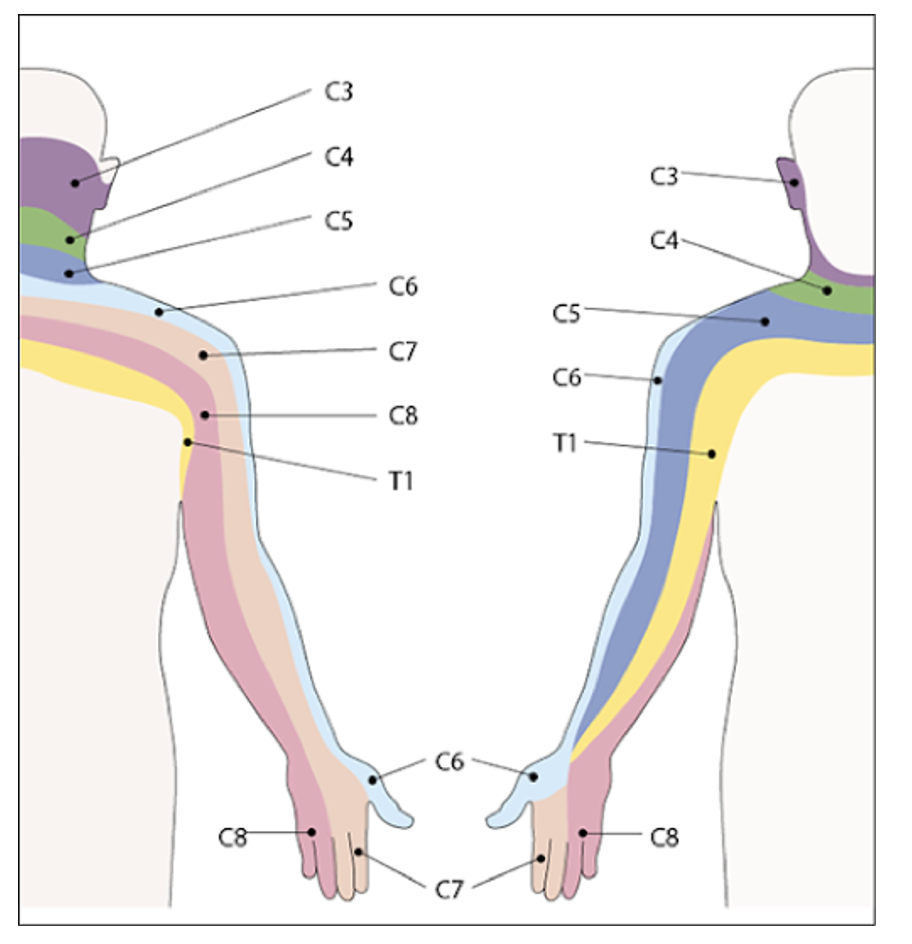
This will achieve numbing of the proximal and lateral upper extremity. Its effects can be inconsistent on C8-T1, therefore distal forearm and ulnar nerve distributions may not be adequately anesthetized
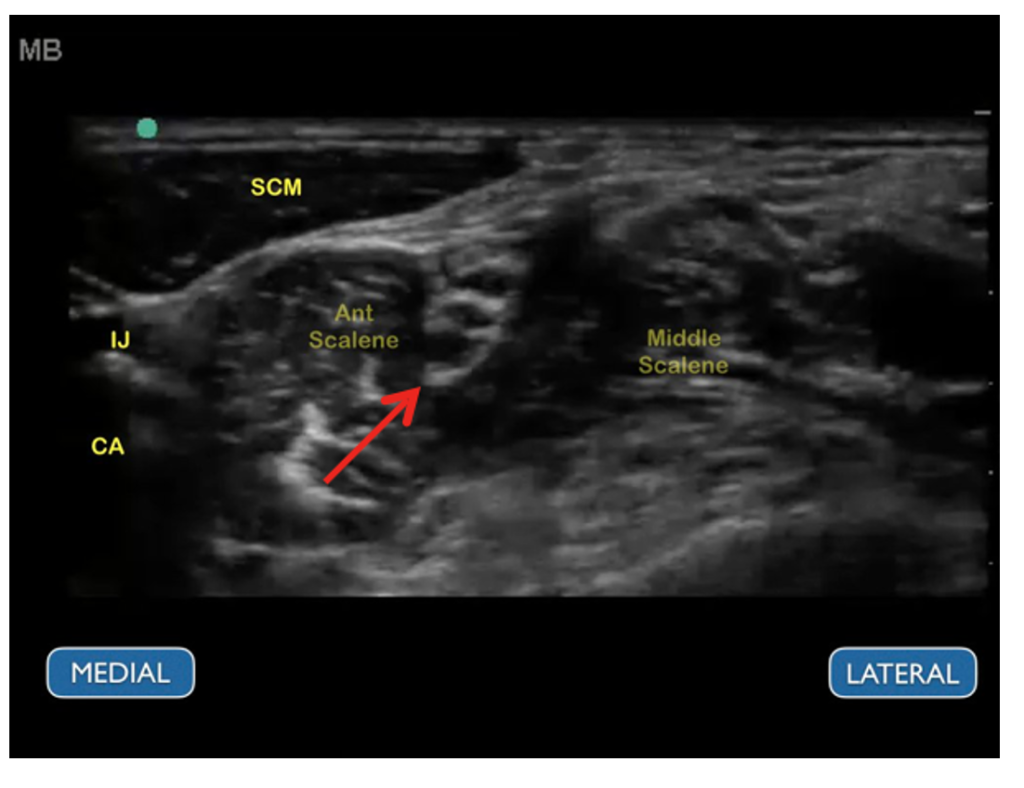
-
The vertically stacked brachial plexus trunks (red arrow) have a “stoplight” appearance in the interscalene groove between the anterior and middle scalene muscle bellies.
-
Image source (red arrow added): https://www.acepnow.com/article/how-to-perform-ultrasound-guided-interscalene-nerve-blocks/
-
Technique:
- The patient should be supine with the head turned 30-45 degrees away from the side to be blocked
- Using the linear transducer in transverse orientation, locate the brachial plexus trunks in the interscalene groove, this can be done by two methods:
-
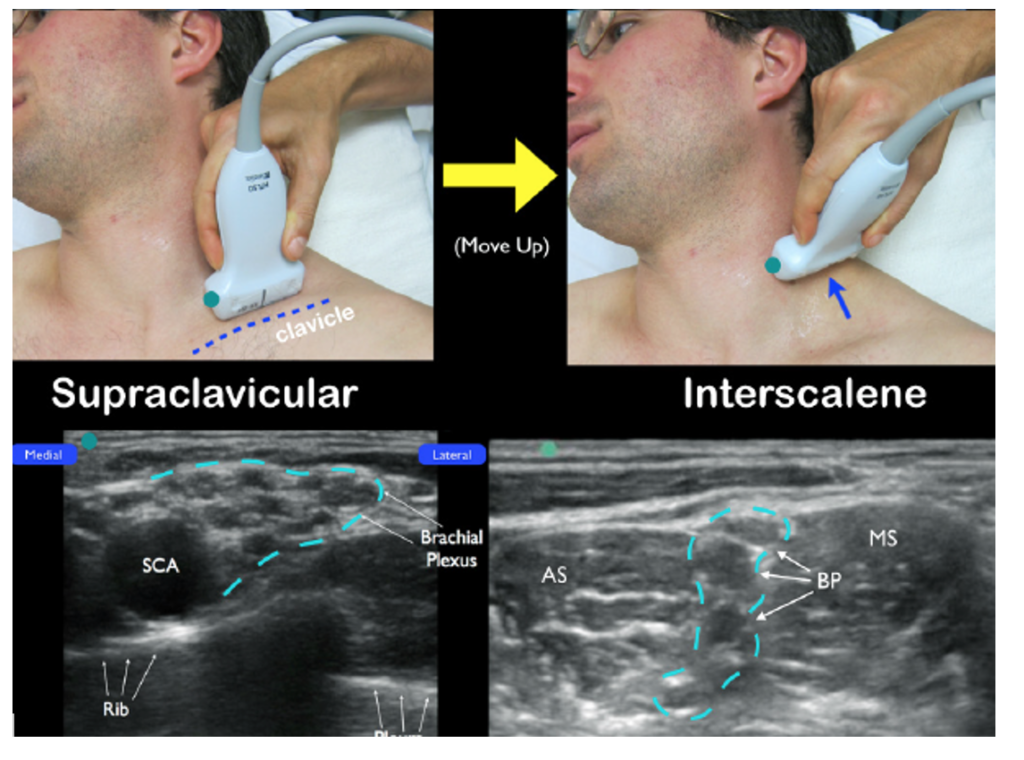
- Method A: Starting in the supraclavicular fossa, locate the subclavian artery and the “bundle of grapes” of the brachial plexus there and move cephalad until the “stoplight” appears.
-
Image source: https://www.acepnow.com/article/how-to-perform-ultrasound-guided-interscalene-nerve-blocks/
-
- Method A: Starting in the supraclavicular fossa, locate the subclavian artery and the “bundle of grapes” of the brachial plexus there and move cephalad until the “stoplight” appears.
-
-
Method B: Starting on the anterolateral neck at the level of the larynx, move the probe laterally until the scalene and “stoplight” come into view. The carotid artery and internal jugular vein should be visible medial to the anterior scalene.
-
Image source: https://www.acepnow.com/article/how-to-perform-ultrasound-guided-interscalene-nerve-blocks/
-
-
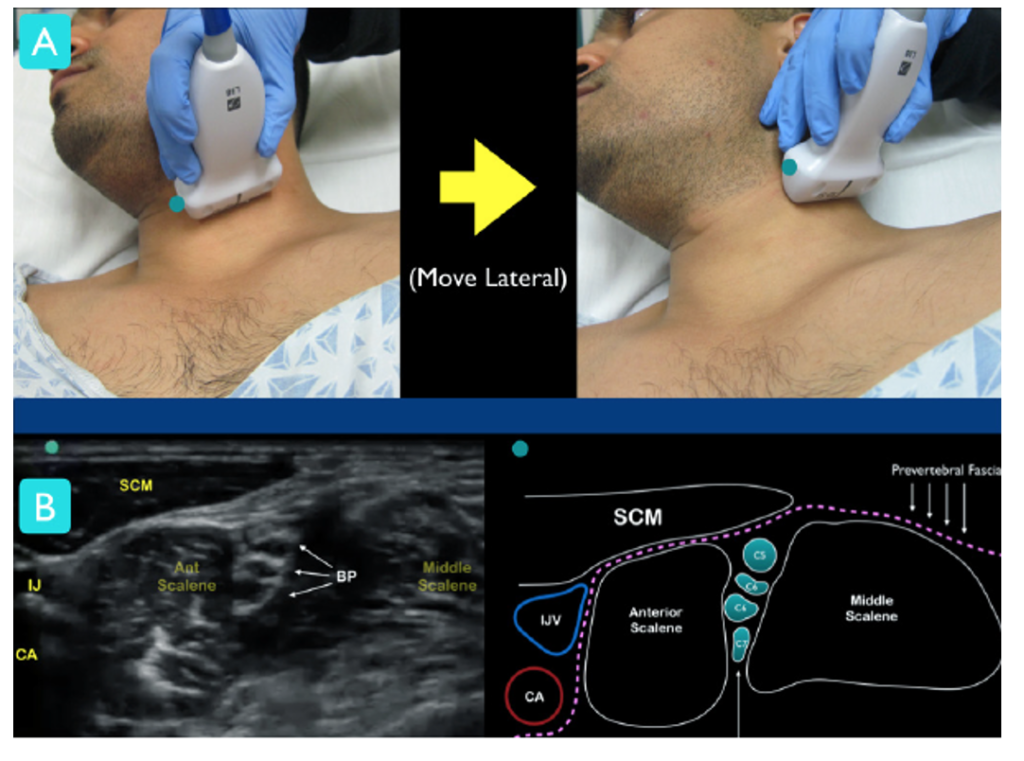
- Use color doppler to help distinguish brachial plexus from nearby vascular structures
- Insert the block needle using an in-plane approach, with the needle entering posterolaterally, moving anteromedially towards the interscalene groove
- First, hydrodissect with a small amount of normal saline under ultrasound visualization to ensure the needle tip is in the correct space in the interscalene groove (i.e. through the prevertebral fascia but not within a muscle belly)
- Inject local anesthetic through the prevertebral fascia to bathe the brachial plexus, ensuring not to get too close to the nerves so as not to inject anesthetic intraneurally
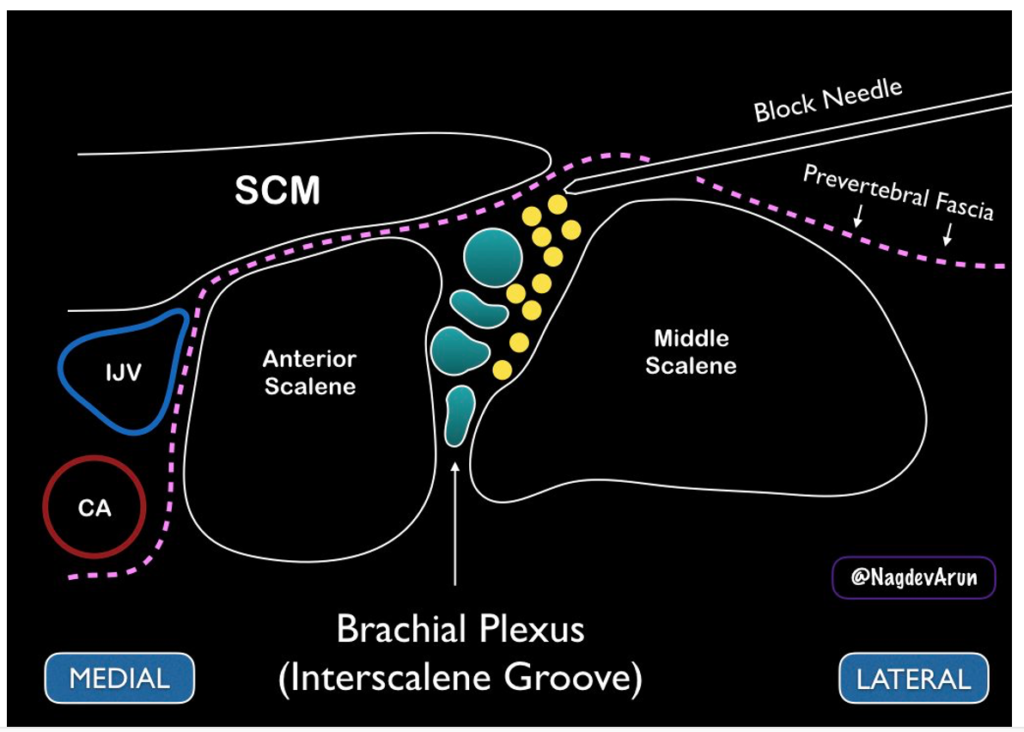
-
- Image source: https://www.acepnow.com/article/how-to-perform-ultrasound-guided-interscalene-nerve-blocks/
Pearls and Pitfalls:
- For more distal upper extremity analgesia (e.g. distal humerus or distal radius fractures) interscalene block may not be as effective as other brachial plexus block approaches (i.e. supraclavicular or axillary).
- Complications include: hematoma, transient hemidiaphragmatic paralysis via involvement on the phrenic nerve, Horner syndrome, recurrent laryngeal nerve paresis, vertebral artery injection, epidural injection, pneumothorax
- To reduce risk of complications, limit anesthetic dose to 10-20 ccs of lidocaine with epinephrine or other short-acting agent.
Sources:
- Blaivas, M., Adhikari, S. and Lander, L. (2011), A Prospective Comparison of Procedural Sedation and Ultrasound‐guided Interscalene Nerve Block for Shoulder Reduction in the Emergency Department. Academic Emergency Medicine, 18: 922-927. doi:10.1111/j.1553-2712.2011.01140.x
- Carmody, K., Moore, C. L., & Feller-Kopman, D. J. (2011). Handbook of critical care and emergency ultrasound. New York: McGraw-Hill Medical.
Excellent information, thank you
Minor typo, in the description of technique for method A, I believe it is meant to say to move “cephalad’ rather than caudal, after identifying the ‘bunch of grapes’
Thanks
Thank you! Corrected!