Background & Pathophysiology:
- An inflammatory colitis caused by fecal impaction
- Marked distension and increased intraluminal pressure leads to ischemic pressure necrosis of the colonic wall and compromise of vascular supply and mucosal perfusion
- Risk of progression to colonic perforation and peritonitis
- Multiple areas of ulceration occur adjacent to the fecaloma; most commonly in the rectosigmoid colon
Diagnosis:
- Lab findings are non-specific – may reveal increased WBC and/or acute phase reactants
- Increased lactate and anion gap metabolic acidosis should raise concern for ischemia and/or perforation
- Supine and erect chest & abdominal radiographs are needed to eval for intraperitoneal free air under the diaphragm, dilated loops of bowel, and air-fluid levels
- CTAP with IV contrast will reveal dilation of the sigmoid colon, colonic wall thickening, thickened rectum, presence of fecal impaction/fecaloma, and/or pericolonic fat stranding
- If extraluminal bubbles of gas or abscess are visualized, this suggests perforation has already occurred.
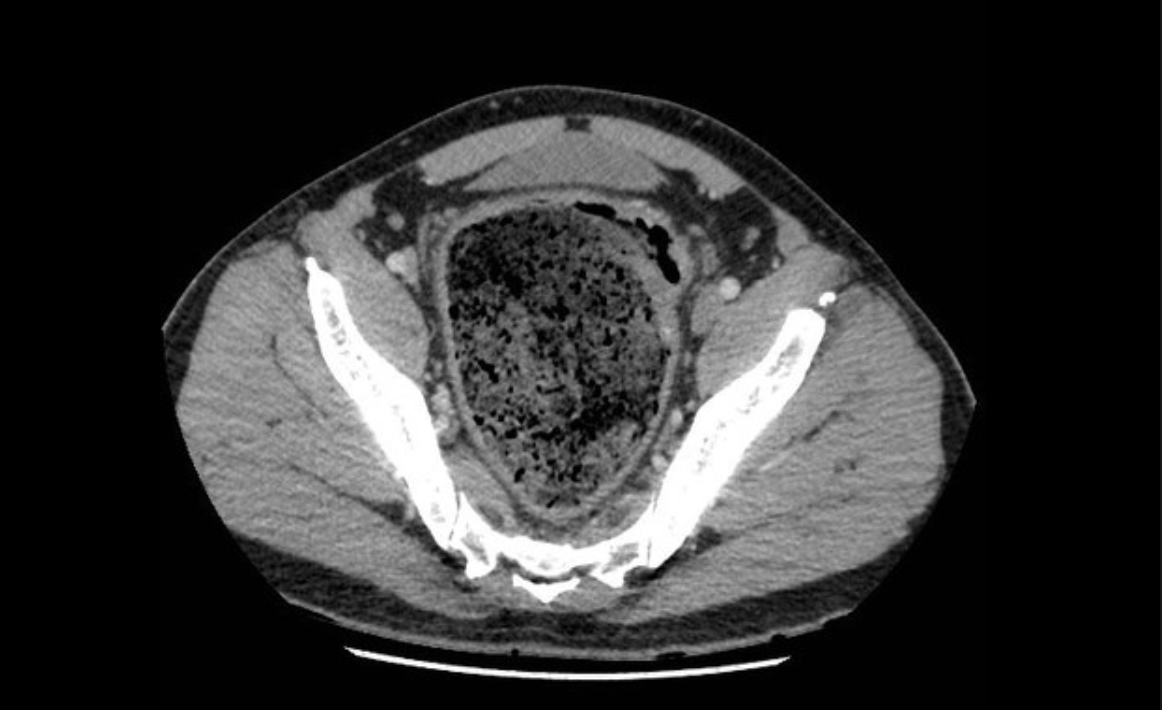
Clinical Presentation:
- Typically elderly patients with chronic constipation; especially those with dementia, nursing home, or bedbound
- Younger patients with psychiatric conditions, patients with chronic opioid use, pediatric patients with severe constipation are also be at risk
- Can present sub-acutely with complaints of constipation (acute on chronic), generalized or localized (LLQ) abdominal pain, urinary retention
- Patients who have perforation may present in extremis with signs of peritonitis and sepsis
Management:
- Joint management with gastroenterology and surgical services
- Stable patients may undergo aggressive bowel regimen with laxatives, enemas, and disimpaction
- GI Endoscopically guided disimpaction may be necessary
- Operative indications: perforation, large segments of bowel involvement, or failure of conservative management
- If fecal impaction is not relieved, colonic perforation with peritonitis and decompensation can occur.
- Treat aggressively with IVF, antibiotics (covering gram negative and anaerobic organisms), and rapid transfer to the OR to resect the affected colon
- A 32-60% mortality rate has been reported when stercoral colitis is associated with perforation!
- Patients with stercoral colitis should be admitted for decompression of the bowel and close monitoring
Pearls:
- Stercoral colitis is an uncommon but potentially fatal complication of chronic constipation
- A high index of suspicion is necessary and should be considered in all patients who present with abdominal pain and constipation, particularly in the elderly
- Active co-management and care coordination with medicine, gastroenterology, and general surgery
- While conservative treatment with bowel regimens and disimpaction may prevent progression, there is a significant potential for perforation
- Imaging: CTAP is the modality of choice for diagnosis
- If starting with plain radiographs, supine & erect films or decubitus are needed to evaluate for free air (multi-view supine x-rays are inadequate) – ensure appropriate views are ordered
References:
- Morano C, Sharman T. Stercoral Colitis. In: StatPearls. StatPearls Publishing; 2021. Accessed August 17, 2021. http://www.ncbi.nlm.nih.gov/books/NBK560608/
- Hudson J, Malik A. A fatal faecaloma stercoral colitis: a rare complication of chronic constipation. BMJ Case Reports. Published online September 3, 2015:bcr2015211732. doi:10.1136/bcr-2015-211732
- Heffernan C, Pachter HL, Megibow AJ, Macari M. Stercoral Colitis Leading to Fatal Peritonitis: CT Findings. American Journal of Roentgenology. 2005;184(4):1189-1193. doi:10.2214/ajr.184.4.01841189
- Naseer M, Gandhi J, Chams N, Kulairi Z. Stercoral colitis complicated with ischemic colitis: a double-edge sword. BMC Gastroenterol. 2017;17(1):129. doi:10.1186/s12876-017-0686-6
- Proulx E, Glass C. Constipation-Associated Stercoral Colitis: Pediatric Emergency Care. 2018;34(9):e159-e160. doi:10.1097/PEC.0000000000001600
- Tajmalzai A, Najah DM. Stercoral colitis due to massive fecal impaction: a case report and literature review. Radiol Case Rep. 2021;16(8):1946-1950. doi:10.1016/j.radcr.2021.04.067
- Weerakkody, Y. Stercoral colitis. 1/22/22. https://radiopaedia.org/articles/stercoral-colitis