Definition: Fractures occurring at or proximal to the surgical neck of the humerus
Epidemiology
- Cause of over 150,000 annual Emergency Department (ED) visits in the US
- Most common fracture affecting the shoulder girdle in adults
- 80% of all humeral fractures (Rockwood 1996)
- 5% of all fractures presenting to the ED (Vachtsevanos 2014)
- Commonly affects elderly women
- Women account for 70% of cases
- Second most common (after distal radius/ulna fractures) upper extremity fracture in patients age 65 yrs and older
Mechanism
- Half of all proximal humerus fractures occur at home with a majority occurring after a fall on level ground
- Older patients (60 yrs and older)
- Low energy trauma, usually fall from a standing height
- Fall onto an outstretched hand with extended elbow
- Younger patients
- High energy trauma, including fall from a height, motor vehicle accidents, sports or assaults
- Direct blows to the arm
- Older patients (60 yrs and older)
Physical Exam
- Diffuse soft tissue swelling and ecchymosis
- Swelling may be absent in obese patients
- Loss of the normal convex contour of the shoulder
- Presence of an anterior or posterior bulge may suggest a dislocation
- Open fractures – rare, however usually present on the medial aspect of the upper arm adjacent to the axilla
- Neurovascular Exam – the axillary nerve and artery are at highest risk of injury. Rarely the brachial artery and brachial plexus may be injured.
- Sensation – assess for hypoesthesia over the lateral aspect of the proximal arm
- Motor function – palpate the deltoid as the patient attempts to actively extend, abduct and flex the shoulder
- Axillary Artery
- Vascular injury more common in elderly patients
- Assess radial pulse and capillary refill of affected arm with comparison to contralateral side
- Assess for the presence of an expanding hematoma
Neer Classification:
- Depends on number of fragments, degree of displacement and presence of dislocation
- Based on four anatomical fracture segments:
- Greater Tuberosity
- Lesser Tuberosity
- Head of Humerus (articular surface)
- Humeral Shaft
- Displaced Fracture: fracture with greater than 1 cm of displacement and less than 45 degrees of angulation from anatomic position (Carofino 2013)
- One Part: Nondisplaced fracture, irrespective of number of fragments
- Two Part: One segment is displaced, either the greater tuberosity, the lesser tuberosity or humeral head
- Three Part: Displacement of one tuberosity and the surgical neck
- Four Part: All four segments (both tuberosities, the articular surface, and the humeral shaft) displaced
- Valgus Impacted Four-Part: head of humerus is rotated into valgus posture and driven down between the tuberosities
- Criticism of Neer Classification:
- Low inter- and intra- observer reliability
- Definition of displacement arbitrarily defined by Neer at time of publication without evidentiary support
- Unable to differentiate between the types of minimally displaced fractures
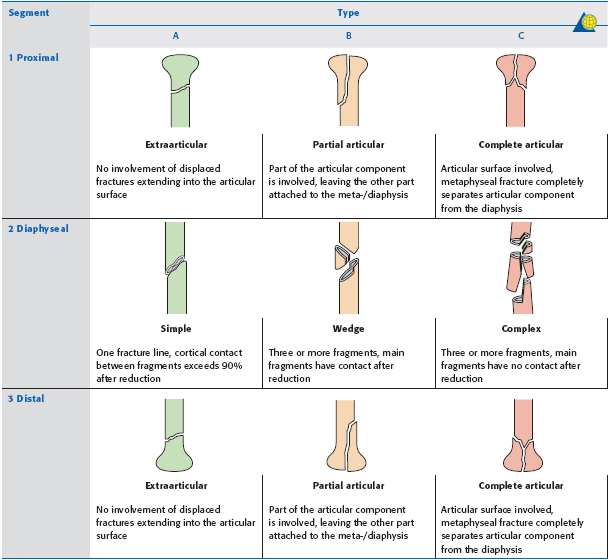
AO/OTA Classification
- Based on fracture location and the presence of impaction, angulation, translation, comminution, or dislocation
- Each fracture type is further subgrouped according to displacement, valgus or varus angulation of the humeral head, comminution and the presence and direction of glenohumeral joint dislocation
- Type A: extra-articular, unifocal, associated with a single fracture line, lowest avascular necrosis (AVN) risk
- A1: greater tuberosity fracture
- A2: surgical neck fracture with metaphyseal impaction
- A3: surgical neck fracture without metaphyseal impaction
- Type B: extra-articular, bifocal, associate with two fracture lines, higher AVN risk
- B1: surgical neck fracture with metaphyseal impaction and a displaced fracture of either the greater or lesser tuberosity
- B2: nonimpacted surgical neck fracture with a displaced fracture of either the greater or lesser tuberosity
- B3: surgical neck fracture with a displaced fracture of either the greater or the lesser tuberosity and glenohumeral dislocation
- Type C: articular fracture, involving either the humeral head or anatomic neck, most severe, highest AVN risk
- C1: Anatomic neck fracture with slight displacement
- C2: Anatomic neck fracture with marked displacement
- C3: Anatomic neck fracture with glenohumeral dislocation
Neer Classification
Imaging
- Radiographs: AP, Scapula Y, and Axillary view
- Additional Views:
- Grashey view (true AP): AP Oblique view allowing for better evaluation of glenohumeral joint and position of humeral head in relation to the joint space
- Modified Velpeau view: modification of axillary view for patients unable to abduct arm
- Additional Views:
- CT Scan: generally not obtained in ED unless suggested by Orthopedics
- Indications: evaluate extent of comminution, displacement of lesser and greater tuberosity fragments, assessment of humeral head and glenoid relationship
Avascular Necrosis of Humeral Head
- Ascending branch of the anterior circumflex humeral artery (ACHA) is the primary source of vascular supply
- Disrupted by fractures through the anatomic neck
- Posterior circumflex humeral artery (PCHA) provides perfusion through the posteromedial proximal humeral metaphysis and becomes predominant source of vascular supply when ACHA is disrupted
- Certain fracture patterns are high risk for disruption of PCHA and therefore ischemia of humeral head:
- Distal metaphyseal extension of the head fragment < 8mm
- Disruption of medial hinge between the humeral head and shaft
- Certain fracture patterns are high risk for disruption of PCHA and therefore ischemia of humeral head:
Management
- Nonoperative Management:
- Nondisplaced or minimally displaced fractures
- 85% of proximal humerus fractures (Quillen 2004)
- Immobilization with a cuff, sling or shoulder immobilizer
- Close Orthopedic follow-up to confirm acceptable alignment and fracture stability
- Early Range of Motion exercise: decreases the risk of developing adhesive capsulitis
- Active range of motion exercises of wrist and hand within 2 weeks of injury
- Displaced fractures: Orthopedic consultation for evaluation and operative planning.
- Non-operative management typically considered in elderly patients with minimal functional demands, patients not fit for surgery
- Complications: malunion, subacromial impingement, osteoarthritis and rotator cuff deficiency
- Nondisplaced or minimally displaced fractures
- Operative Management
- The use of operative treatment in displaced fractures is increasing, due to concern for improved functional outcome. However, in the literature, no clear benefit has been found.
- PROFHER Trial: in patients with displaced fractures involving the surgical neck, no significant difference in clinical outcome in patients treated operatively versus non-operatively (Handoll 2015)
- Cochrane Review: no significant difference in patient functional outcome at 1 year. Those who underwent operative treatment required additional surgical intervention. (Handoll 2012)
- Selection of surgical approach depends on: classification, involvement of tuberosity or surgical neck, patient age and expected level of activity.
- Closed Reduction and Percutaneous Pinning (CRPP)
- Indications: 2- and 3- part surgical neck fractures
- Complications: fixation failure, intra-articular pin migration, axially nerve injury
- Contraindications: head-split fractures, fracture-dislocations, complex fractures in the elderly
- Open Reduction and Internal Fixation (ORIF)
- Indications: Neer 2-, 3- and 4- part fractures with rotation greater than 45 degrees or displacement greater than 5mm (or 1 cm, depending on source), Head splitting fractures in younger patients (Part of humeral head dislocates and the unfractured part remains attached to the shaft)
- Preferred in younger patients due to good bone quality and joint preservation
- Complications: impingement, screw penetration, screw cutout and fixation loss.
- Complication rate as high as 34% (Neviaser 2015).
- Hemiarthoplasty
- Previously the gold standard for treatment of complex fractures
- Satisfactory pain relief but inconsistent functional outcome (Kontakis 2008)
- Indications:
- Displaced 4- part fractures and fracture-dislocations at high risk for osteonecrosis
- Fractures with inadequate reduction or fixation, fractures with vascular compromise
- Complications: infection, dislocation, intraoperative or periprosthetic fractures and rotator cuff dysfunction
- Previously the gold standard for treatment of complex fractures
- Reverse Total Shoulder Arthroplasty
- Indications: Alternative treatment for displaced 4-part fractures and nonreconstructible tuberosities
- Procedure of choice in patients over 70 with complex fractures (Boyle 2013)
- Closed Reduction and Percutaneous Pinning (CRPP)
- The use of operative treatment in displaced fractures is increasing, due to concern for improved functional outcome. However, in the literature, no clear benefit has been found.
- Prognosis: Overall prognosis is good. Poor prognosis is associated with: older age, presence of displacement, 3- and 4- Part Neer fractures, Type C AO Fractures
Take Home Points
- Proximal humerus fractures commonly occur in patients over age 65 (especially women) secondary to a fall on an outstretched had
- The presence of displacement, defined as fractures with greater than 1 cm of displacement and less than 45 degrees of angulation, often determines operative versus non-operative management plan
- The most common injury pattern (Neer One-part fracture) is treated with sling, early range of motion exercises and Orthopedic follow-up
References
Allen, Deborah. “Proximal Humerus Fractures.” Orthobullets. 2 Oct. 2015. Web. 2 Nov. 2015.
Boyle M., et al. Functional outcomes of reverse shoulder arthroplasty compared with hemiarthroplasty for acute proximal humeral fractures. JShoulder Elbow Surg 2013 Jan;22(1):32-7. PMID: 22652065
Carofino BC, Leopold SS. Classifications in brief: the Neer classification for proximal humerus fractures Clin Orthop Relat Res. 2013 Jan;471(1):39-43 PMID: 22752734
Fractures. In Classifications and Scores of the Shoulder (pp. 119-142). Berlin: Springer Berlin Heidelberg; 2006.
Handoll H., et al. Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev. 21012;12 PMID: 23235575
Handoll H., et al. The ProFHER trial – a pragmatic multicenter randomized controlled trial evaluating the clinical effectiveness and cost-effectiveness of surgical compared with non-surgical treatment for proximal fracture of Humerus in adults. Health Technol Assess. 2015 Mar;19(24):1-280. PMID: 25822598
Ip D. Orthopedic Traumatology – A Resident’s Guide. 2nd ed. Berlin-Heidelberg:Springer Verlag; 2009.
Kontakis G, et al. Prosthetic replacement for proximal Humerus fractures. Injury. 2008 Dec;39(12):1345-58. PMID: 19036360
Neviaser RJ., et al. Proximal Humerus Fractures: pin, plate or replace. Instr Course Lect. 2015;64:203-14. PMID: 25745906
Quillen D et al. Acute Shoulder Injuries. Am Fam Physician. 2004; 70(10): 1947-1954. PMID: 15571061.
Rockwood CA. Jr, Green DP, Bucholz RW, Heckman JD. Fractures in Adults. 4th ed. Philadelphia, Pa: Lippincott-Raven; 1996.
Vachtsevanos L., et al. Management of proximal humerus fractures in adults. World J Orthop. 2014 Nov 18;5(5):685-93. PMID: 25405098