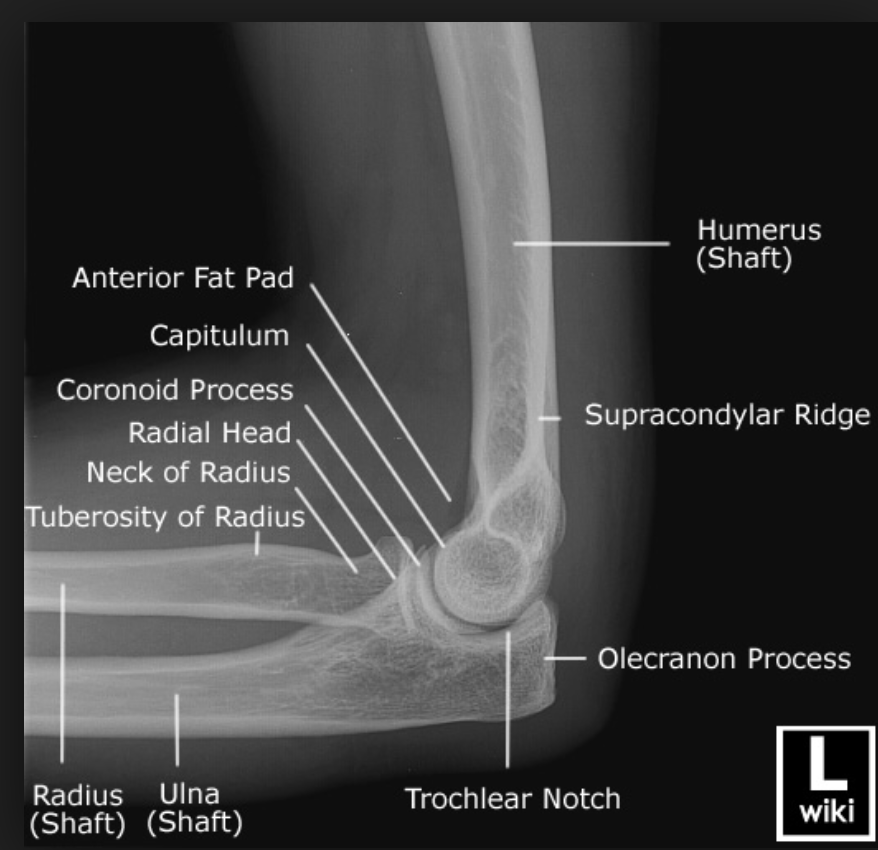
X-ray of Normal Elbow Anatomy – http://www.wikiradiography.net
Definition: Disarticulation of ulna from humerus.
Mechanism:
- Elbow joint is very stable and requires a significant force to dislocate- most common mechanism is fall onto outstretched arm
- Posterior: elbow hyperextension, arm abduction, and forearm supination together cause movement of the olecranon posteriorly (ex: falling onto an extended arm)
- Anterior: direct force to posterior forearm while elbow is in flexion
- Most dislocations have an associated injury to capsuloligamentous stabilizers that progresses from lateral to medial, with the anterior band of medial collateral ligamental (MCL )being the last to be injured and is most often intact after injury (exceptions: trans-olecranon fracture dislocations, coronoid fractures)
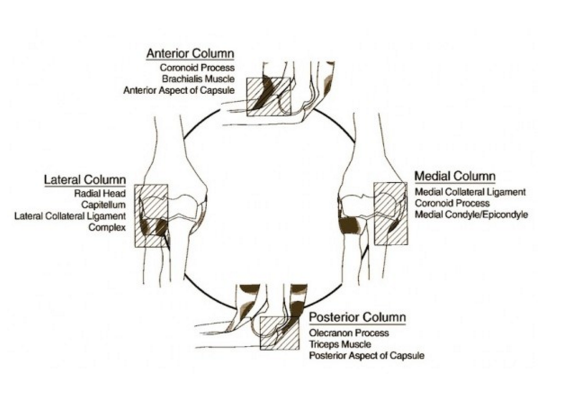
Elbow Anatomy – www.lifeinthefastlane.com
Epidemiology:
- Most common dislocation in children
- Second most common dislocation site in adults (shoulder is #1)
- Accounts for 10-25% of elbow injuries (Kuhn 2008)
- Posterolateral dislocations are most common
- Highest incidence in 10-20 year-old males associated with sports injuries
- Up to 50% have associated fracture
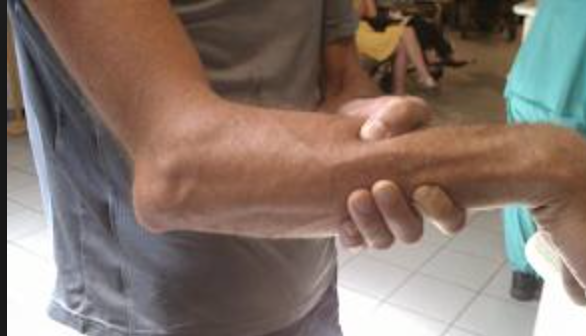
Posterior Dislocation – http://sportsrehabcoach.com/
Physical Exam:
- Varying degrees of gross swelling, deformity and instability
- Posterior: elbow is flexed with prominence of olecranon- on palpation olecranon is displaced from plane of epicondyles (see image below)
- Anterior: elbow held in full extension, upper arm appears shortened with forearm held in supination and elongated
- Perform neurovascular exam prior to manipulation and radiographs
- Most commonly injured vessel: Brachial Artery- more common with anterior and open dislocations (see neurovascular anatomy image below)
- Median and ulnar nerve are most susceptible to damage
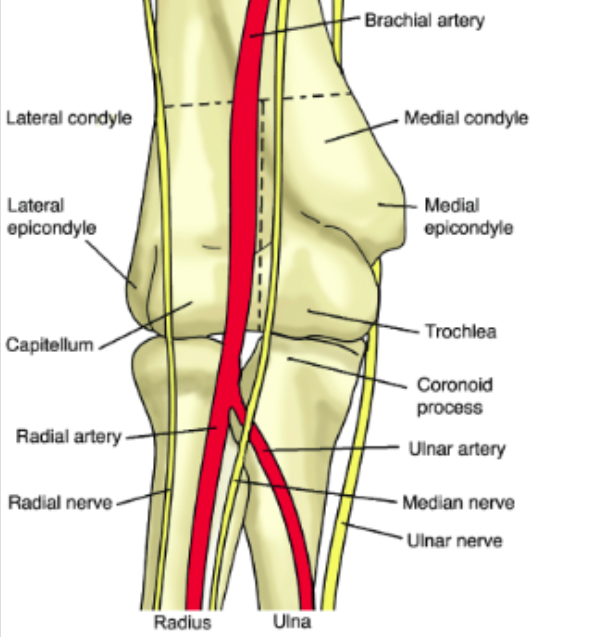
Neurovascular Anatomy – http://accessemergencymedicine.mhmedical.com/
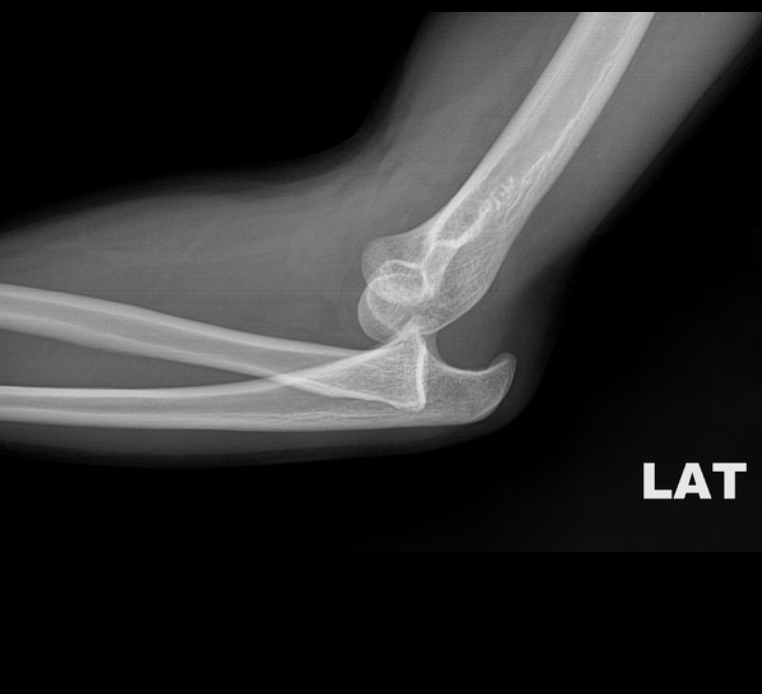
X-Ray: Posterior Dislocation – http://radiopaedia.org/
X-ray Findings:
- Assess orientation of dislocation (ulna relative to humerus)
- Recommended views: AP, lateral
- Additional views: Oblique- will help assess periarticular bony involvement
- Look for associated fractures:
- Medial/lateral epicondyle (12-34%)
- Radial head (5-10%)
- Coronoid process (5-10%)
- Terrible Triad: posterior dislocation with radial head and coronoid process fractures
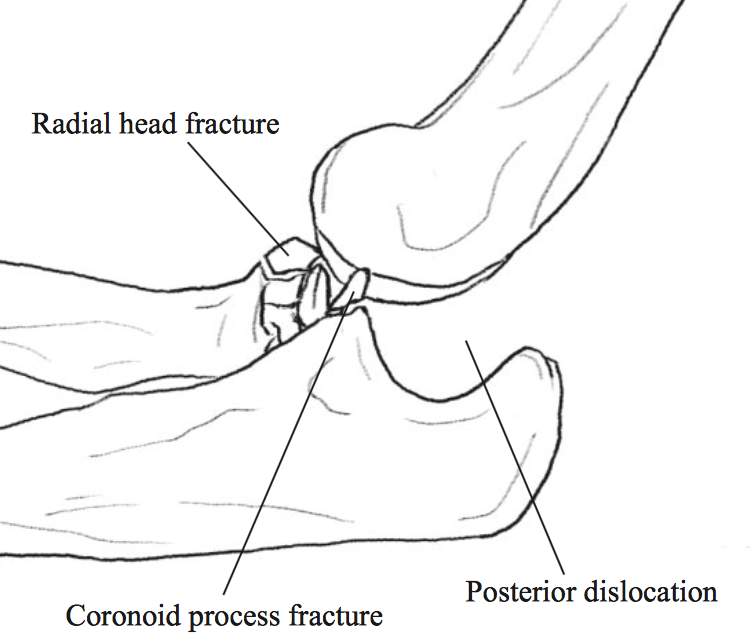
“Terrible Triad” (Xiao 2015)
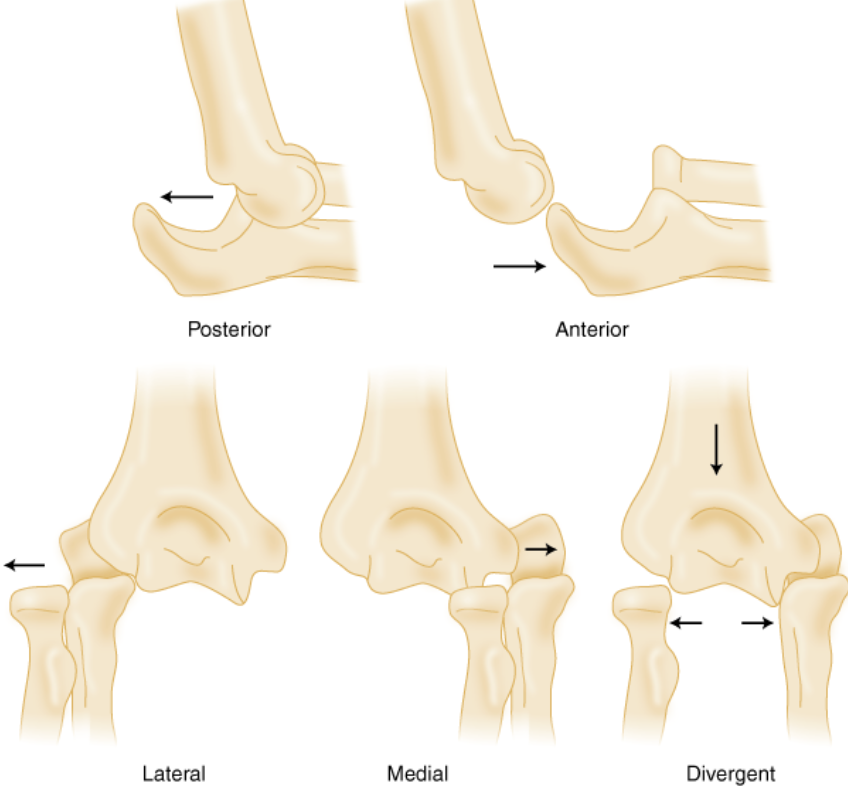
Dislocation Classification – http://www.fprmed.com/
Dislocation Classification:
- Simple vs complex:
- Simple: dislocation
- Complex: dislocation with fracture
- Classify according to the direction of displacement of ulna relative to humerus
- Posterior, posterolateral, posteromedial, lateral, medial, anterior
ED Management:
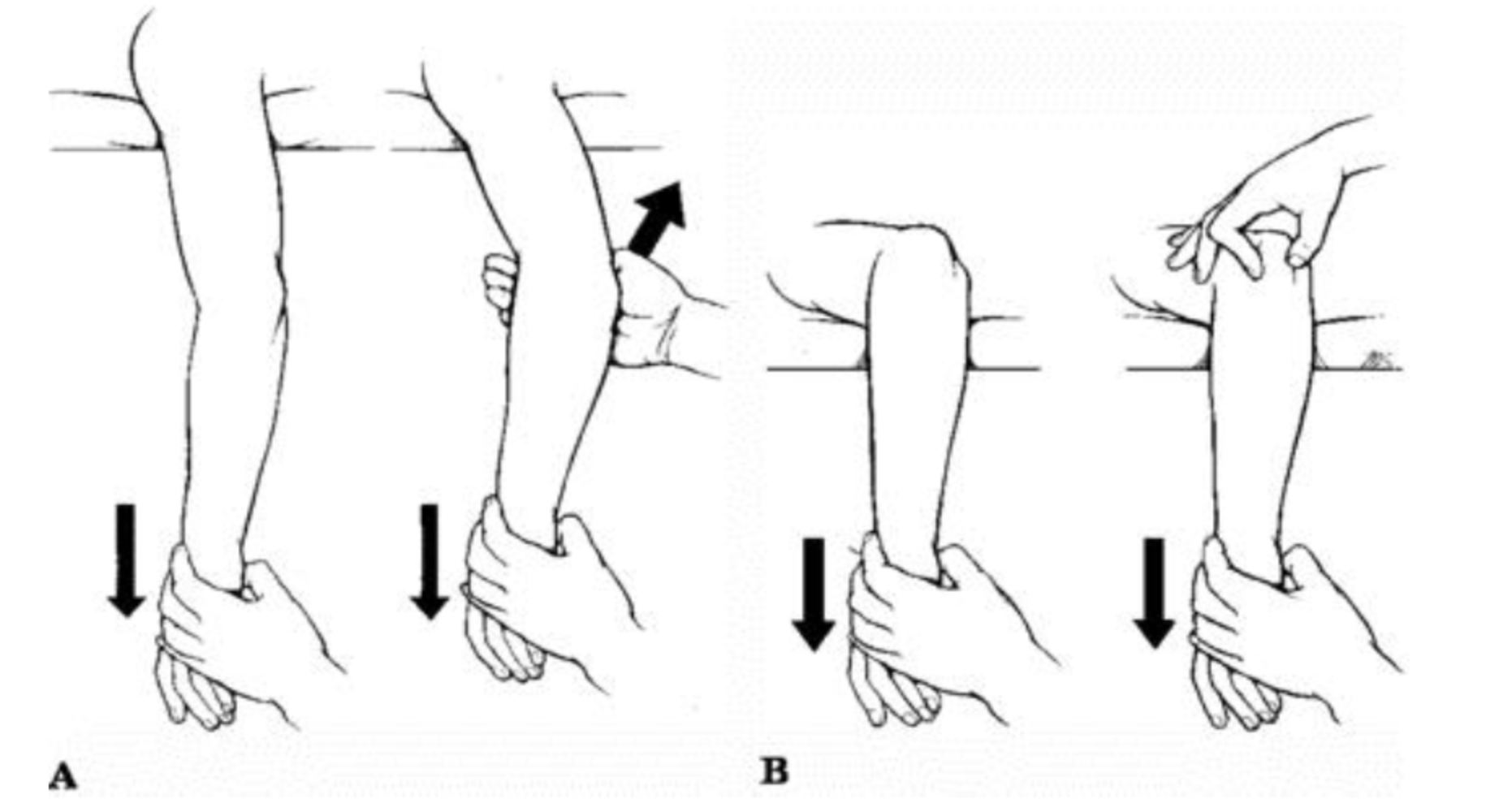
Parvin’s (A) and Meyn & Quigley (B) Reduction Techniques (Egol 2010)
- Emergent orthopedic consult for any patient with concern for vascular damage (loss of pulse), neurological deficits (loss of sensation, contractures) or open dislocation/fracture
- Simple Dislocation
- Closed reduction: correction of medial or lateral displacement followed by longitudinal traction and flexion
- Parvin’s method: patient lies prone with entire upper extremity hanging off the bed, downward traction is applied to the wrist for a few minutes—> olecranon slips distally, arm is then lifted gently (Method A)
- Meyn & Quigley method: forearm hangs off of bed, gentle downward traction is applied to wrist, olecranon is guided with opposite hand (Method B)
- Assess range of motion after reduction (instability can be appreciated with elbow extension)
- Immobilize in long arm posterior splint with elbow in 90 degrees of flexion for 1-2 week with orthopedics follow up as outpatient within 1 week for repeat radiographs
- A recent multi-center study suggests that early mobilization may be superior to immobilization with better functional outcomes at 6 weeks, but comparable functional outcomes at 1 year (Iordens 2015)
- Prolonged immobiization (>3 weeks) is associated with poor functional outcomes, pain and contractures (Melhoff 1988)
- If persistently unstable after reduction, splint, obtain repeat radiogrpahs to ensure elbow joint and fractures (if any) are in stable position and will need immediate orthopedics followup in the next 3-5 days for repeat radiographs and will likely need a more pronlonged immobilization course with splinting for 2-3 weeks and a hinged splint for up to 4 weeks (Ahmed 2015)
- Closed reduction: correction of medial or lateral displacement followed by longitudinal traction and flexion
- Complex Dislocations:
- Most will need operative management, however, reduction and splinting may be definitive management for patients with minimally or non-displaced radial head fracture
- Patients who elect for non-op management must be made aware of potential for instability of joint and future restriction of range of motion
Prognosis:
- Recurrent dislocations are uncommon (incidence is increased when terrible triad is present)
- Stiffness of joint is common
- Immobilization should not exceed 2 weeks
- Volkmann contracture (claw hand): Can develop in the pressence of massive soft tissue swelling. Consider checking compartment pressures
Take Home Points:
- Three complications of elbow dislocations that must be appreciated and require operative management: neurovascular compromise, associated fractures, open fractures
- Simple, uncomplicated dislocations can be treated with closed reduction, splinting and orthopedic follow up in 1-2 weeks
References:
Ahmed I, Mistry J. The Management of acute and chronic elbow instability. Orthop Clin North Am. 2015 Apr;46(2):271-80. PMID: 25771321
Aiyer A, Moore D. Elbow Dislocation. (2015, May 22) [Ortho Bullets] Retrieved from: http://www.orthobullets.com/trauma/1018/elbow-dislocation.
Egol K et al. Handbook of Fractures. Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health, 2010.
Iordens GI. et al. Early mobilisation versus plaster immobilisation of simple elbow dislocations: results of the FuncSiE multicentre randomised clinical trial. Br J Sports Med. 2015 Jul 14. [Epub ahead of print] PMID: 26175020
Kuhn MA, Ross G. Acute elbow dislocations. Orthop Clin North Am 2008; 39: pp. 155-161. PMID: 18374806
Mehlhoff TL et al. Simple dislocation of the elbow in the adult: Results after closed treatment. J Bone Joint Surg Am 1988 Feb;70(2):244-9.PMID: 3343270
Najarian, Sandra L. Chapter 171. Forearm and Elbow Injuries. In: Tintinalli JE, Stapczynski J, Ma O, Cline DM, Cydulka RK, Meckler GD, T. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7e. New York, NY: McGraw-Hill; 2011