Maternal Alloimmunization: Development of antibodies to the Rh antigen
- Occurs when Rh (-) mother is pregnant with Rh (+) fetus and is exposed to fetal blood
- During subsequent pregnancies with Rh (+) fetus, maternal antigens can attack fetal blood leading to hemolytic disease of the newborn (hydrops fetalis)
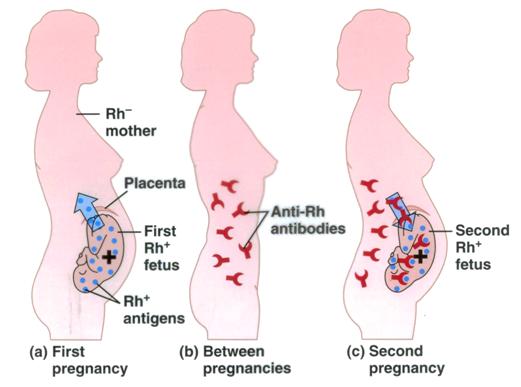
Rh D Isoimmunization – intranet.tdmu.edu.ua
Epidemiology
- Prior to development of Anti-D immunoglobulin, 16% of Rh negative women were alloimmunized after delivery Rh positive fetuses
- Anti-D immunoglobulin was developed in 1960’s and prevalence of alloimmunization decreased to 1-2% when administrated after delivery
- Prevalence decreased to 0.1-0.3% after administration in first trimester (Moise, Up to Date)
Cost Effectiveness of Anti-D immunoglobulin
- Anti-D immunoglobulin created from human plasma and is in limited supply
- ED Costs
- Drug cost
- Cost of type and screen testing
- Cost in prolonged treatment time
Evidence of Alloimmunization in First Trimester
- Fetal/Maternal blood mixing occurs in 7% of first trimester pregnancies (Cohen 1964)
- RhD antigen found to develop in fetus as early as 6 weeks (Urbaniak 1998)
- In a 1960’s study of healthy Rh negative men who were given Rh positive blood, it was demonstrated that approximately 0.1 mLof RH-positive blood is needed to undergo alloimmunization (Stern 1961)
- Mean volume of fetal cells in maternal circulation at 8 weeks approximately 0.33ml (Urbaniak 1998)
- Incidence of fetomaternal hemorrhage in patients with threatened abortion (Von Stein 1992)
- Used Kleihauer-Betke test to detect fetal cells in maternal circulation
- Study population was women <20 weeks with
- Threatened Ab: 11% fetomaternal hemorrhage
- No Threatened Ab: 4% fetomaternal hemorrhage
- There are similar studies supporting the presence of maternal exposure to fetal blood but limited evidence that antibodies formed in maternal circulation in 1st trimester resulting from this exposure (Jabara 2003)
Evidence of Anti-D Immunoglobulin preventing sensitization
- Single randomized control examining efficacy of anti-D immunoglobulin in 1st trimester (Visscher 1972)
- 57 pregnant Rh (-) women undergoing spontaneous abortion in 1st trimester
- 29 were given placebo and rest were given anti-D immunoglobulin
- No evidence of alloimmunization at 3 or 6 month follow up
- No further randomized control trials have been done to show anti-D immunoglobulin prevents alloimmunization
Expert Recommandations
- American College of Emergency Physicians (ACEP) (Hahn 2012)
- Recommendation
- Treatment with anti-D immunoglobulin is recommended in 1st trimester bleeding
- Level B recommandation (based off moderate clinical certainty)
- Acknowledges controversy of this topic and agrees that data is limited
- States that their conclusion is based mostly on theory/observational studies as opposed prospective/experimental studies
- Recommendation
- American Congress of Obstetricians and Gynecologists (ACOG) (ACOG Bulletin 1999)
-
- In regards to administration of anti-D immunoglobulin in 1st trimester pregnancy, the guideline states, “no evidence-based recommendation can be made,” and that “Rh D alloimmunization apparently attributable to threatened abortion is exceedingly rare.”
- Recommendations
- Anti-D immunoglobulin should be given in ectopic pregnancies in the 1st trimester (Level A)
- Anti-D immunoglobulin should be given for threatened abortions with significant bleeding (Level C)
Take Home Points
- Fetal/Maternal transfusion has been well documented during 1st trimester pregnancy
- Alloimmunization in the 1st trimester can occur in theory but has not been clinically proven
- There is an absence of high-quality data demonstrating that anti-D immunoglobulin prevents alloimunization in 1st trimester
- No evidence based recommendation for administration can be made at this time. The best recommendation is to follow the standard practice in your area
Read More
Core EM: Episode 86.0 – Anti-D Immunoglobulin (RhoGam) in Early Pregnancy
References
Moise K Prevention of Rh(D) alloimmunization in pregnancy. Up To Date Link
Von Stein AG et al. Fetomaternal hemorrhage in threatened abortion. Obstet Gynecol 1992; 79(3): 383-386. PMID: 1738519
Cohen F et al. Mechanisms of isoimmunization. I. The transplacental passage of fetal erythrocytes in homospecific pregnancies.” Blood 1964; 23: 621-646. PMID: 14142502
Stern K et al. Experimental isoimmunization to hemoantigens in man. J Immunol 1961; 87: 189-198. Link
Urbaniak SJ The scientific basis of antenatal prophylaxis. Br J Obstet Gynaecol 1998; 105 Suppl 18: 11-8. PMID: 9863973
Jabara S, Barnhart KT. Is Rh immune globulin needed in early first-trimester abortion? A review. Am J Obstet Gynecol 2003; 188(3): 623-627. PMID 12634631
Visscher RD, Visscher HC. Do Rh-negative women with an early spontaneous abortion need Rh immune prophylaxis? Am J Obstet Gynecol 1972; 132(2):158-165 PMID: 4623673
Hahn SA et al. Clinical policy: Critical issues in the initial evaluation and management of patients presenting to the emergency department in early pregnancy. Ann Emerg Med 2012; 60(3): 381-390. PMID: 22921048
ACOG Practice Bulletin. Prevention of Rh D alloimmunization. Int J Gynecol Obstet 1999; 66: 63-70. PMID: 10458556