Definition: An abdominal aortic aneurysm (AAA) is localized dilation (> 3 cm) of the aorta caused by a weakening involving all three layers (intima, media and adventitia) of the aortic wall. It most commonly develops distal to the renal arteries.
Epidemiology:
- Uncommon in patients < 50 yo
- Found in 2-5% of men > 50 yo
- It is more common:
- In men than women
- In patients with coronary artery disease (CAD) or peripheral arterial disease (PAD)
- Patients with a family history of AAA
- Smokers
- Up to 50% of AAA in patients < 65 occur in women
- Mortality
- 30-40% with open aortic repair
- 20-25% with endovascular repair
Presentation
Unruptured Aneurysm
- Signs and Symptoms
- Most AAAs are asymptomatic until expansion or rupture occurs
- Pain is a common symptom when symptoms are present
- Abdominal, back and/or flank pain
- Acute pain associated with a AAA can mimic renal colic
- Acute pain may be an ominous sign of impending rupture
- Physical Exam
- Large aneurysms may be found on routine abdominal examination as pulsatile abdominal masses
- May be limited secondary to patient body habitus and size of aneurysm
- Abdominal bruits are uncommon findings
- Complications of unruptured AAAs
- Thromboembolic: lower extremity ischemia
- Direct compression of adjacent structures (duodenum, ureters etc)
Ruptured Aneurysm
- Classic Triad: Pain, hypotension and a pulsatile abdominal mass. Often will only see one or two features of the triad
- Symptoms
- Pain is the most common symptom
- Abdominal, back and/or flank
- Typically acute in onset, severe and can radiate to the chest, back or groin
- Acute onset of pain in a patient with a AAA should be assumed to be secondary to rupture
- Syncope (or near-syncope) is common though hemodynamic compensation may result in near-normalization of blood pressure
- Pain is the most common symptom
- Physical Exam
- Large, palpable abdominal mass
- Aortic pulsation may be felt (may be absent if blood pressure is low)
- Hypotension
- Seen in 50% of ruptures on presentation (Gaughan 2009, Rose 2001)
- Late finding suggestive of impending hemodynamic collapse and death
- Tachycardia may be variably present
- Many patients are on beta-blockers at baseline
- Blood in the abdomen can stimulate vagal responses leading to lower than expected heart rate
- AAA Variants
- Aortoenteric fistula
- Definition: AAA rupture into the GI tract that can be either primary (from an unrepaired AAA) or secondary (after prior aortic repair)
- Consider diagnosis in any patient with a known AAA or prior repair who presents with GI bleeding
- Can see both hematemesis and melena as the aortoenteric fistula commonly connects the AAA to the duodenum
- Patients will typically experience rapid, massive exsanguination. Aortoenteric fistula has a very high morbidity and mortality
- Aortocaval fistula
- Definition: Periaortic inflammation leads to a connection between the AAA and the adjacent vena cava.
- Free rupture of the AAA will present in same way as any ruptured AAA
- Formation of a large arteriovenous (AV) fistula may occur if there is no external AAA leak
- Signs and Symptoms (Cinara 2005)
- Palpable mass (80-90%)
- Abdominal bruit (75%)
- Palpable thrill (25%)
- Aortoenteric fistula
Differential Diagnosis
- Aortic Dissection
- Ureteric Colic
- Pancreatitis
- Intestinal ischemia
- Bowel obstruction
- Diverticulitis
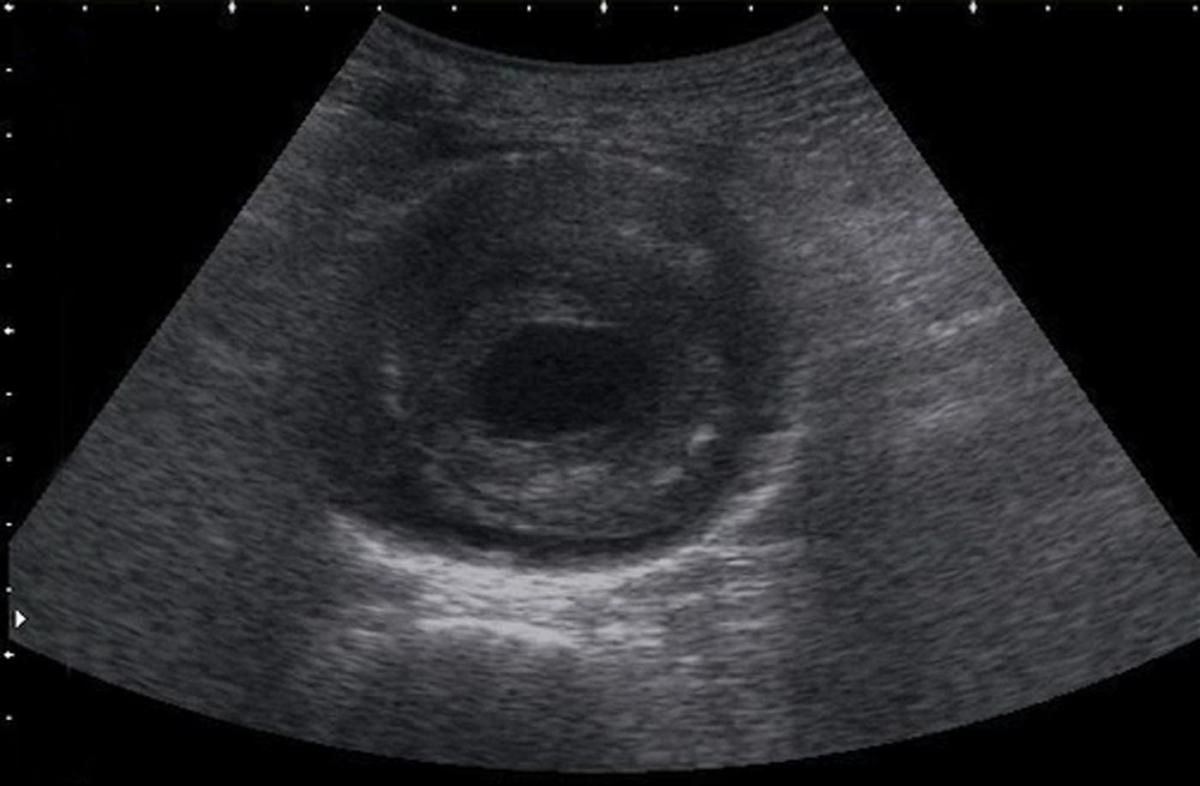
US Short Axis: Abdominal Aortic Aneurysm (emergencyultrasoundteaching.com)
Diagnostics
- Patients with ruptured aneurysms will often be diagnosed based on clinical presentation alone.
- Ultrasound
- Sensitivity for detecting AAA approaches 100% (Lederle 2003)
- Detection of AAA rupture
- Presence of free intraperitoneal fluid confirms rupture
- Rupture may be retroperitoneal or small leading to a false negative US for free fluid
- Advantages
- Allows for rapid evaluation of the aorta as a cause for shock in the undifferentiated patient while resuscitation is ongoing
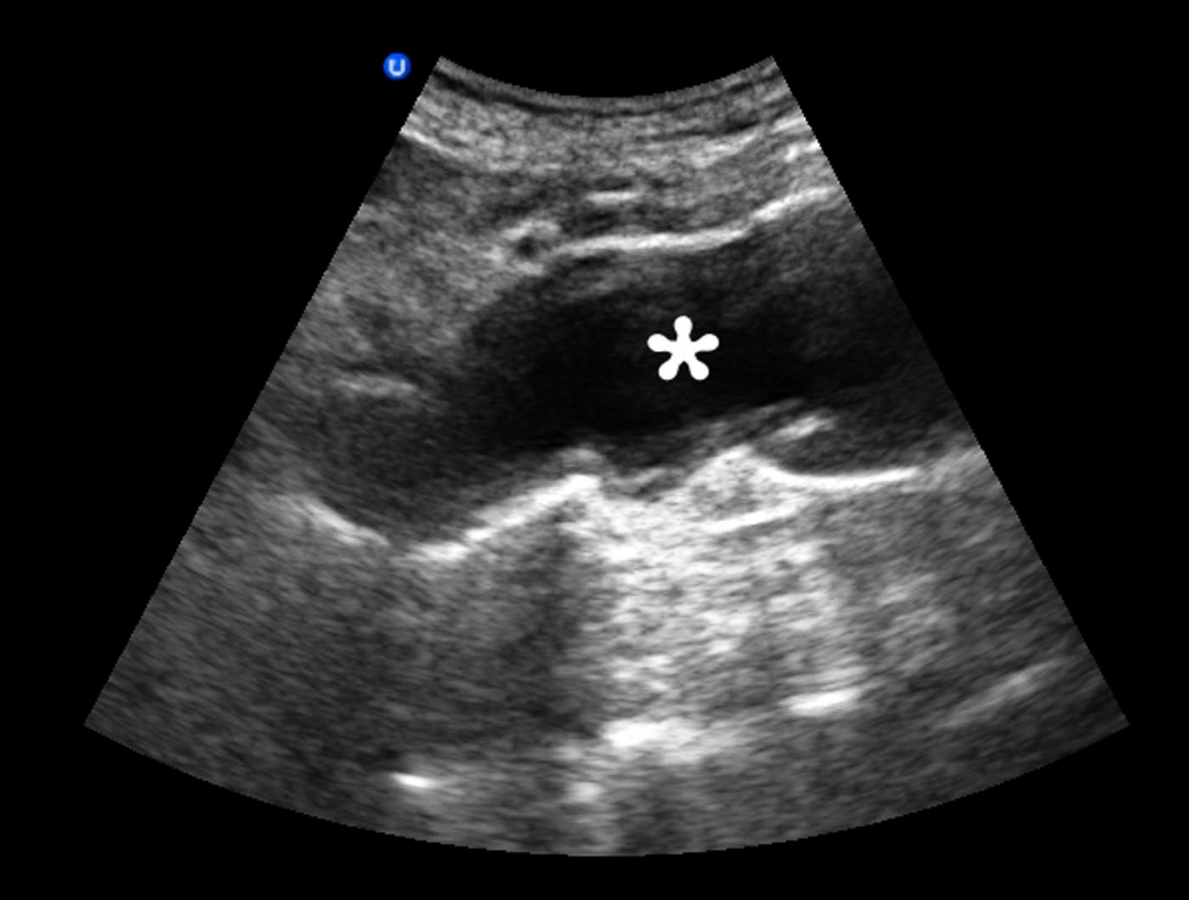
US Transverse Axis: Abdominal Aortic Aneurysm (emergencyultrasoundteaching.com)
- Obviates the need for the patient to be transported to the radiology department for imaging
- Can provide alternative explanations for the patient’s presentation
- Allows for rapid evaluation of the aorta as a cause for shock in the undifferentiated patient while resuscitation is ongoing
- Limitations
- Prone to both technical (ultrasonographer skills) and interpretive error
- Visualization of the aorta can be limited by obesity or the presence of bowel gas
- Not as sensitive for detecting rupture
- CT Scan
- Abdominal CT has a sensitivity and specificity approaching 100% for both diagnosis of AAA as well as rupture (Hermsen 2004)
- Addition of IV contrast can delineate the patent lumen of the AAA from the mural thrombus but is not
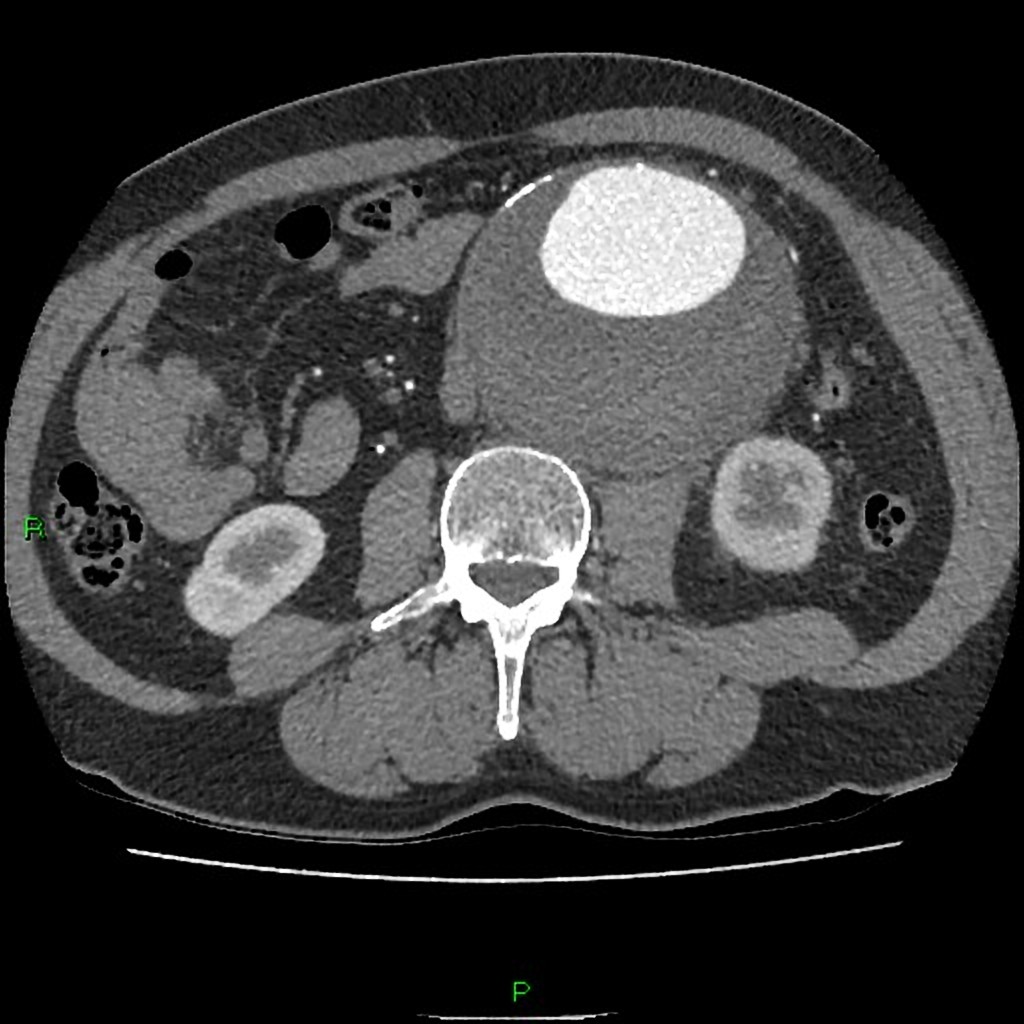
Infrarenal AAA on CT with Contrast (Case courtesy of Dr Derek Smith, Radiopaedia.org. From the case rID: 36556)
necessary for identification of aneurysm or hemorrhage
- More sensitive than US for detecting retroperitoneal hemorrhage of AAA
- CT also helpful in identifying alternative diagnoses
Management
Regardless of vital signs, patients with ruptured AAA should be considered unstable and should be aggressively resuscitated. A ruptured AAA has a mortality rate > 80%. (Adam 1999)
Basics: ABCs, Large bore (> 16 gauge) IV X 2, Supplemental O2 (if needed), Cardiac Monitor + Immediate Surgical Consultation for repair
Aggressive Volume Resuscitation in Hypotensive patients
- Target systolic blood pressure of 90-100 mm Hg pre-operatively
- Exact target unknown
- Over-resuscitation may contribute to increased bleeding from dilutional coagulopathy
- Under-resuscitation harmful as prolonged hypotension can lead to end-organ damage (myocardial infarction, renal failure) and cardiac arrest
- Start with administration of uncrossmatched blood
- Activate massive transfusion protocol as patients often have large transfusion requirements
- Consider administration of a 1:1:1 (PRBC:FFP:Platelets) ratio of blood products
- Administer reversal agents for anticoagulant use if indicated
Take Home Points
- Consider ruptured AAA in patients (especially those > 50 years of age) with unexplained hypotension, back or abdominal pain
- All ruptured AAAs should be considered unstable regardless of vital signs as rapid deterioration is common
- A ruptured AAA is 100% fatal without surgical or endovascular intervention. Mobilize your surgical colleagues early
Read More
Bessen HA, Poffenberger CM: Abdominal Aortic Aneurysm, in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2010, (Ch) 86: p 1129-1140.
References
Adam DJ et al. Community and hospital outcome from ruptured abdominal aortic
aneurysm within the catchment area of a regional vascular surgical service. J Vasc Surg
1999; 30:922-928. PMID: 10550191
Cinara IS et al: Aorto-caval fistulas: A review of eighteen years experience. Acta Chir Belg 2005; 105:616-620. PMID: 16438071
Gaughan M et al. Emergency abdominal aortic aneurysm presenting without haemodynamic shock is associated with misdiagnosis and delay in appropriate clinical management. Emerg Med J 2009; 26:334-339. PMID: 19386866
Hermsen K, Chong WK. Ultrasound evaluation of abdominal aortic and iliac aneurysms and mesenteric ischemia. Radiol Clin North Am 2004; 42:365-381. PMID: 15136022
Lederle FA: Ultrasonographic screening for abdominal aortic aneurysms. Ann Intern
Med 2003; 139:516-522. PMID: 24957320

If old pat suffering from abdominal pain without hypotension and on bedside us is negative for intra peritoneal fluid it is safe to send pat for ct scan to confirm the retro peritoneal rupture.?..
I think that’s where you have to go but I would be cautious and possibly accompany patient if CT far from ED.