The Case
CC
Shortness of breath two hours after arthroscopy
HPI
75 yo F presents with shortness of breath 2 hours after arthroscopy. Patient states she had an outpatient arthroscopy of R shoulder that was uneventful but felt short of breath at discharge, about 30 min post-procedure, that is now progressively worsening. Denies chest pain, fevers/chills, cough, nausea/vomiting.
PMH / PSH
PMH: arthritis, htn
Meds: amlodipine, nsaids
ALL: nkda
PSH: s/p R shoulder arthroscopy (2 hours ago)
Soc: never smoker, denies all illicit substances
FHx: non-contributory
Physical Exam
VS: HR 120s RR 32 O2sat 85% RA Tc 98.6 FS 102
GEN: appears to be in respiratory distress, speaking 2 word sentences, aox3
Cor: +s1, s2, regular but tachycardic
Pulm: cta b/l
Abd: soft, nt, nd, +b.s.
Extr: +2 pulses b/l, no LE edema, arthroscopy site appears clean, dry and intact
Labs
Labs: pending
EKG: sinus tachycardia
See CXR
Media
Questions
-
What is the most likely diagnosis?
As seen in the CXR, there is elevation of the right hemidiaphragm compared to the left. The patient has hemidiaphragmatic paralysis on the right causing shortness of breath.
-
What is the most likely mechanism that caused the condition?
Patient just underwent right shoulder arthroscopy likely with interscalene regional anesthesia that blocked the phrenic nerve causing ipsilateral hemidiaphragmatic paralysis.
-
What is the best management of this patient?
The management of unintentional phrenic nerve block is largely supportive. Patients should also be reassured that their respiratory distress will resolve when the block wears off, which can be up to 18 hours depending on anesthetic used. Support the patient’s breathing with supplemental oxygen; for some patients this may be enough. If the patient continues to be in respiratory distress, they may require non-invasive mechanical ventilation or even intubation. In our patient, her symptoms rapidly resolved with supplemental oxygen via facemask. She was admitted to the step-down unit for observation with complete resolution of hemidiaphragmatic paralysis overnight and discharged the next day.
More Info
Interscalene block and its complications
The interscalene block is a popular brachial plexus block used for shoulder arthroscopies. It can often prevent the use of general anesthesia as well as provide post-operative pain management. Analgesia with the interscalene block will be sustained for 8-10 hours and up to 18 hours depending on the type of local anesthetic used2.
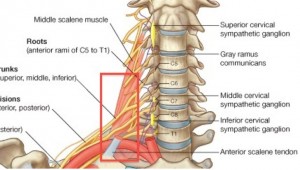 The brachial plexus courses out of the cervical spine into the upper extremities. Going from proximal to distal, the brachial plexus divides into roots (comprised of the individual nerve roots rising from the cervical spine), trunks, divisions, cords and branches. Roots of the brachial plexus form 3 trunks, the superior, middle, and inferior trunks, which traverse between the anterior and middle scalene muscles in the neck. The interscalene block is performed at the level of the C6 vertebral body, which is the same level as the cricoid cartilage. Anesthesia injected into the interscalene groove aims to block nerves C5 to C7 or the superior and middle trunks that innervate the muscles of the shoulder. The inferior trunk, C8 and T1, is less reliably anesthetized. Therefore, any procedure below the elbow may require further regional anesthesia.
The brachial plexus courses out of the cervical spine into the upper extremities. Going from proximal to distal, the brachial plexus divides into roots (comprised of the individual nerve roots rising from the cervical spine), trunks, divisions, cords and branches. Roots of the brachial plexus form 3 trunks, the superior, middle, and inferior trunks, which traverse between the anterior and middle scalene muscles in the neck. The interscalene block is performed at the level of the C6 vertebral body, which is the same level as the cricoid cartilage. Anesthesia injected into the interscalene groove aims to block nerves C5 to C7 or the superior and middle trunks that innervate the muscles of the shoulder. The inferior trunk, C8 and T1, is less reliably anesthetized. Therefore, any procedure below the elbow may require further regional anesthesia.
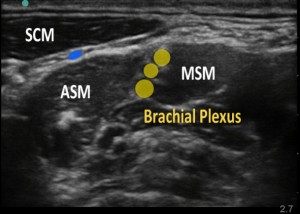 There are several important structures around the interscalene space that may cause unintended complications to this block. First, as the presented patient experienced, there is almost 100% incidence of ispilateral phrenic nerve block with interscalene blocks8. The phrenic nerve (composed of contributions from C3 to C5) lies on the ventral aspect of the anterior scalene muscle (blue dot on ASM). Anterior spread of local anesthetic is rarely avoidable. Therefore, ipsilateral hemidiaphragmatic paralysis is common in patients receiving interscalene block. Phrenic nerve blocks resulting in hemidiaphragm paralysis can cause significant reduction in pulmonary function. Urmey et al found a 27% decrease in forced vital capacity, 26.4% decreased in forced expiratory volume, 15.4% decrease in peak expiratory flow rate associated with hemidiaphragmatic paralysis7. While most healthy adults would be able to tolerate hemidiaphragmatic paralysis without symptoms, patients with less pulmonary reserve such as the elderly may experience respiratory distress. It is important to consider the patient population when performing interscalene blocks as patients such as the elderly, the morbidly obese, or patients with underlying lung disease e.g. COPD may not be able to tolerate the decrease in pulmonary function.
There are several important structures around the interscalene space that may cause unintended complications to this block. First, as the presented patient experienced, there is almost 100% incidence of ispilateral phrenic nerve block with interscalene blocks8. The phrenic nerve (composed of contributions from C3 to C5) lies on the ventral aspect of the anterior scalene muscle (blue dot on ASM). Anterior spread of local anesthetic is rarely avoidable. Therefore, ipsilateral hemidiaphragmatic paralysis is common in patients receiving interscalene block. Phrenic nerve blocks resulting in hemidiaphragm paralysis can cause significant reduction in pulmonary function. Urmey et al found a 27% decrease in forced vital capacity, 26.4% decreased in forced expiratory volume, 15.4% decrease in peak expiratory flow rate associated with hemidiaphragmatic paralysis7. While most healthy adults would be able to tolerate hemidiaphragmatic paralysis without symptoms, patients with less pulmonary reserve such as the elderly may experience respiratory distress. It is important to consider the patient population when performing interscalene blocks as patients such as the elderly, the morbidly obese, or patients with underlying lung disease e.g. COPD may not be able to tolerate the decrease in pulmonary function.
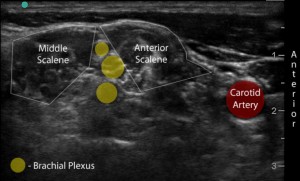 Other lesser-associated potential complications from interscalene blocks include seizure, ipsilateral horner’s syndrome and hoarseness of voice. The carotid artery is just medial to the anterior scalene muscle. If the carotid artery is inadvertently punctured and anesthesia is introduced into the artery, seizures can occur. To suppress seizures, benzodiazepines are preferred4. Just posterior to the carotid artery resides the stellate ganglion, part of the cervical sympathetic chain. Posterior and medial migration of anesthesia can affect the stellate ganglion causing reversible horner’s syndrome (ipsilateral miosis, anhidrosis and ptosis) in about 18% of patients1.
Other lesser-associated potential complications from interscalene blocks include seizure, ipsilateral horner’s syndrome and hoarseness of voice. The carotid artery is just medial to the anterior scalene muscle. If the carotid artery is inadvertently punctured and anesthesia is introduced into the artery, seizures can occur. To suppress seizures, benzodiazepines are preferred4. Just posterior to the carotid artery resides the stellate ganglion, part of the cervical sympathetic chain. Posterior and medial migration of anesthesia can affect the stellate ganglion causing reversible horner’s syndrome (ipsilateral miosis, anhidrosis and ptosis) in about 18% of patients1. 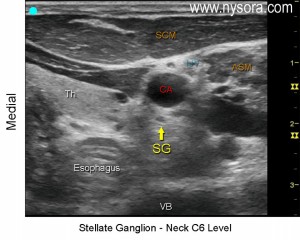 Patients with horner’s syndrome after interscalene block only require reassurance that symptoms will resolve after local anesthesia is metabolize. Of a more serious, but less common occurrence is the blockage of the recurrent laryngeal nerve which courses its way upwards around C7. Blockage of the recurrent laryngeal nerve can cause transient hoarseness, but can also cause respiratory distress if patient has underlying contralateral vocal cord disease6.
Patients with horner’s syndrome after interscalene block only require reassurance that symptoms will resolve after local anesthesia is metabolize. Of a more serious, but less common occurrence is the blockage of the recurrent laryngeal nerve which courses its way upwards around C7. Blockage of the recurrent laryngeal nerve can cause transient hoarseness, but can also cause respiratory distress if patient has underlying contralateral vocal cord disease6.
Pearls:
- Outpatient shoulder arthroscopies often utilize regional blocks, specifically the interscalene brachial plexus block
- There is almost 100% incidence of ipsilateral phrenic nerve block associated with interscalene blocks
- Management for hemidiaphragmatic paralysis secondary to unintentional phrenic nerve block usually only require supportive care and reassurance
References:
- Al-Khafaji JM, Ellias MA, Incidence of horner syndrome with interscalene brachial plexus block and its importance in the management of head injury, Anesthesiology 1986 Jan;64(1):127.
- Blunting, L. V. “Interscalene Plexus Block.” Ultrasound Guided Nerve Block. Ultrasound Guide for Emergency Physicians, 2008. Web. 6 Dec. 2015.
- ECRI and ISMP, “Reducing Complications from Interscalene Blocks.” Reducing Complications from Interscalene Blocks. Pennsylvania Patient Safety Advisory, 4 Dec. 2007. Web. 06 Dec. 2015.
- Neal JM, Mulroy MF, Weinberg GL. American Society of Regional Anesthesia and Pain Medicine checklist for managing local anesthetic systemic toxicity, Reg Anesth Pain Med. 2012 Jan-Feb. 37(1):16-8.
- Neill, Andy. “US Scalene Block for Shoulder Reduction – Emergency Medicine Ireland.” Emergency Medicine Ireland. Emergency Medicine Ireland, 17 Oct. 2011. Web. 06 Dec. 2015.
- Thukral, S, Gupta P, Gupta M, Lakra A, Recurrent laryngeal nerve palsy following interscalene brachial plexus block: How to management and avoid permanent sequelae?, J Anaesthesiol Clin Pharmacol, 2015 Apr-Jun;31(2):282-3.
- Urmey WF, McDonald M, Hemidiaphragmatic paresis during interscalene brachial plexus block: effects on pulmonary function and chest wall mechanics, Anesth Analg, 1992 Mar;74(3):352-7.
- Urmey WF, Talts HK, Sharrock NE, One hundred percent incidence of hemidiaphragmatic paresis associated with interscalene brachial plexus anesthesia as diagnosed by ultrasonography, Anesthesia and Analgesia, 1991; 72(4): 498-503.


1) Paralysis of the hemidiaphragm
2) Complication of regional anesthesia (brachial plexus block) – nervus phrenicus block
3) Since the pathophysiology in the lungs is shunting, oxygen therapy might not be enough, leading to ventilator support until effects of local anesthethics wear off?
Interscene block is the likely regional anesthesia used for the shoulder arthroplasty. The phrenic nerve passes near brachial plexus at target for ISB so some degree of hemiparalysis of diaphragm is expected but usually not clinically significant. I question if this patient has in diagnosed lung or CV disease? Treatment start with positioning seated or recumbent > supine with supplemental O2. If still in distress perhaps mechanical ventilation as above mentioned?
Pleural based wedge shaped opacity (Hampton hump) suggestive of pulmonary infarction, usually indicates embolism