The Case
CC
Chest pain
HPI
50yM no PMH, active smoker presents by ambulance with chest pain. Six hours ago he developed substernal chest pressure and nausea, no vomiting. Pain was moderate and constant, but he had a presyncopal episode 1hr prior and severe worsening of chest pain which led him to call 911. He was given ASA en route.
PMH / PSH
No medications or known PMH
Physical Exam
BP 109/44 | HR 95 | RR 18 | T 98.5F | SpO2 92% RA → 97% 4L NC
GEN: diaphoretic, pale, grimacing, clutching his chest in pain, speaking in incomplete sentences
CV: tachycardic, regular, 3/6 systolic ejection murmur
PULM: CTAB
ABD: soft, non-tender, non-distended
NEURO: no focal deficits, moves all extremities equally
Labs
CBC: 17.6 > 15.4 / 43.9 < 189
BMP: 140 / 4.4 / 107 / 23 / 21 / 1.4 < 139
LFT: 91 / 37 / 90 / 1.6 / 0.0 / 4.2 / 7.5
Troponin: 4.33
VBG: 7.50 / 34.3 / 26.7 Lact 2.95
Media
Questions
-
What are your next steps in management of this patient?
STEMI team was activated and the patient was started on heparin and promptly taken for cardiac catheterization. He had normal coronary arteries but was noted to have severe aortic insufficiency and a dissection flap in the ascending aorta consistent with type A aortic dissection.
-
What additional therapies would you consider administering?
He was started on labetalol and as the patient was being consented for emergent operative repair by CT surgery, he admitted to longstanding and recent crystal meth use. Intraoperatively, an intimal tear was noted 2-3cm above the sinotubular junction with the intimal flap dissecting through the aortic valve; graft repair was performed with good outcome.
More Info
Aortic dissections have a highly variable presentation, which makes diagnosis challenging. It is much rarer than ACS, with an incidence of 5-30 cases per million people, and a high risk of mortality (classically 1-2% increase in mortality with each passing hour) (Hagan 2000). There is no information in the literature regarding the incidence of aortic dissection among cases that present as myocardial infarctions. However, several independent studies reveal the incidence of troponin elevations in aortic dissection to be 12-18% (Davis 2005, Hansson 2012, Leitman 2013) and ST elevations to be 2-8% (Hagan 2000, Davis 2005, Luo 2009, Hirata 2010, Hansson 2012) – both remarkably consistent ranges.
The following table summarizes currently available evidence:
| Symptom | Prevalence in Type A dissections* | Sensitivity or Specificity** | Likelihood Ratio 2002† | Likelihood Ratio 2017** |
| Good for ruling out: | ||||
| Sudden onset of chest pain, maximal at onset | 85-90% | Sensitivity 95.9% | LR- 0.3 | LR- 0.07 |
| Good for ruling in: | ||||
| Ripping, tearing pain | 49% | Specificity 99.7% | LR+ 10.8 | LR+ 42.1 |
| Hypotension | 25% | Specificity 98.7% | – | LR+ 17.2 |
| Syncope / neuro deficit | 13% | Specificity 96.9% | LR+ 33.0 | LR+ 5.3 |
| Aortic insufficiency murmur | 44% | Specificity 97.8% | LR+ 4.9 | LR+ 9.4 |
| Pulse deficit | 19% | Specificity 99.3% | LR+ 2.7 | LR+ 31.1 |
| Other diagnostics: | ||||
| Widened mediastinum on CXR | 63% | Sensitivity 52.4% Specificity 94.9% |
LR- 0.1 LR+ 3.4 |
LR- 0.5 LR+ 10.2 |
| EKG normal / nonspecific changes | 30% / 43% | – | – | – |
| EKG STEMI or ischemic changes | 5% | Sensitivity 21.8% Specificity 87.7% |
– | LR- 0.9 LR+ 1.8 |
| Echo with aortic root dilation | 42% | Sensitivity 60.8% Specificity 93.9% |
– | LR- 0.4 LR+ 10.0 |
* Hagan 2000 (IRAD)
** Ohle 2017
† Klompas 2002
Lessons from this particular case of aortic dissection mimicking myocardial infarction are outlined below. These principles are consistent with a recently published approach (Helman 2017). These small cost-effective changes in a provider’s chest pain initial workflow may increase his/her suspicion for aortic dissection.
Better history taking
- The absence of sudden/maximal intensity at onset has the lowest LR- to rule out aortic dissection.
- “Ripping” or “tearing” chest pain has the highest LR+ to rule in aortic dissection.
- Need for IV narcotics for controlling chest pain should raise suspicion for aortic dissection.
- Ask about obvious risk factors such as hypertension and drug use.
The commotion and diagnostic bias in this particular case led to an incomplete history.
Better examination
- In patients with aortic dissections <40 years old, 50% had Marfan syndrome. Since people may not know they have Marfan syndrome, visually note whether the patient has lanky “Marfanoid” features.
- Take a second and listen for a murmur and feel for radial pulse deficit. Either finding highly specific for aortic dissection.
In this case, a murmur was appreciated on exam but not considered.
The “CP+1” Concept (Helman 2017)
- Any focal neurologic deficit in the setting of acute chest pain is highly specific for aortic dissection.
The patient in this case reported pre-syncope, and a more thorough neurologic examination should have been performed.
Consider your diagnostics
- Although a normal CXR is reassuring based on LR-, one-third of dissections have normal CXRs. Normal CXRs are not reliable for ruling out a dissection.
- ACEP does not recommend relying on D-dimers for workup of aortic dissection. (Diercks 2015)
- Consider point-of-care ultrasound TTE views. Although ACEP does not recommended relying on TTE for diagnosis of aortic dissection (Diercks 2015), it is moderately sensitive but highly specific for aortic dissection if a dissection flap or cardiac tamponade is seen.
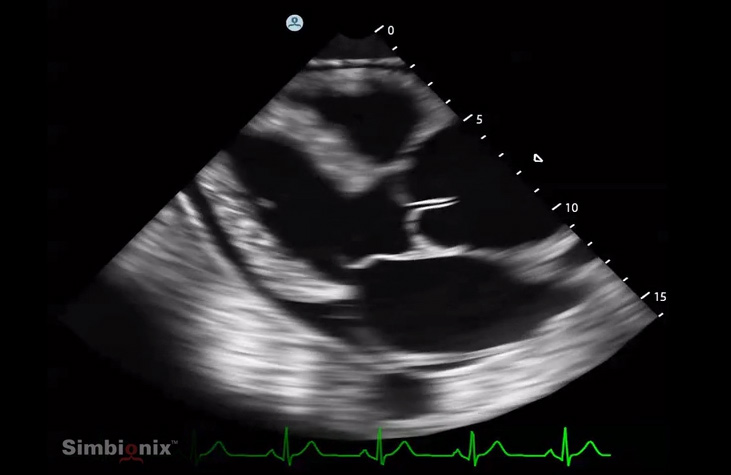
Parasternal long view demonstrating pericardial effusion and enlarged aortic root (top right). http://simbionix.com/simulators/us-mentor/us-library-of-modules/us-bedside-echocardiography/. See also https://youtu.be/Ivrw3M2uJFI?t=2m30s.
These cost-effective clues may increase the provider’s pre-test suspicion for aortic dissection and lead him/her to order CTA for definitive diagnosis.
With regards to therapeutics, in our patient’s case, he received inappropriate anticoagulation. One study noted a 50% complication rate in nine patients with aortic dissection that had been inappropriately anticoagulated – usually increased intraoperative bleeding (Davis 2005). Poor outcomes have also been described from tPA administration for (incorrect) suspicion of acute stroke or acute MI in patients with aortic dissection. Thankfully, our patient did not receive dual antiplatelet agents, received only easily reversible heparin, and suffered no significant complications.
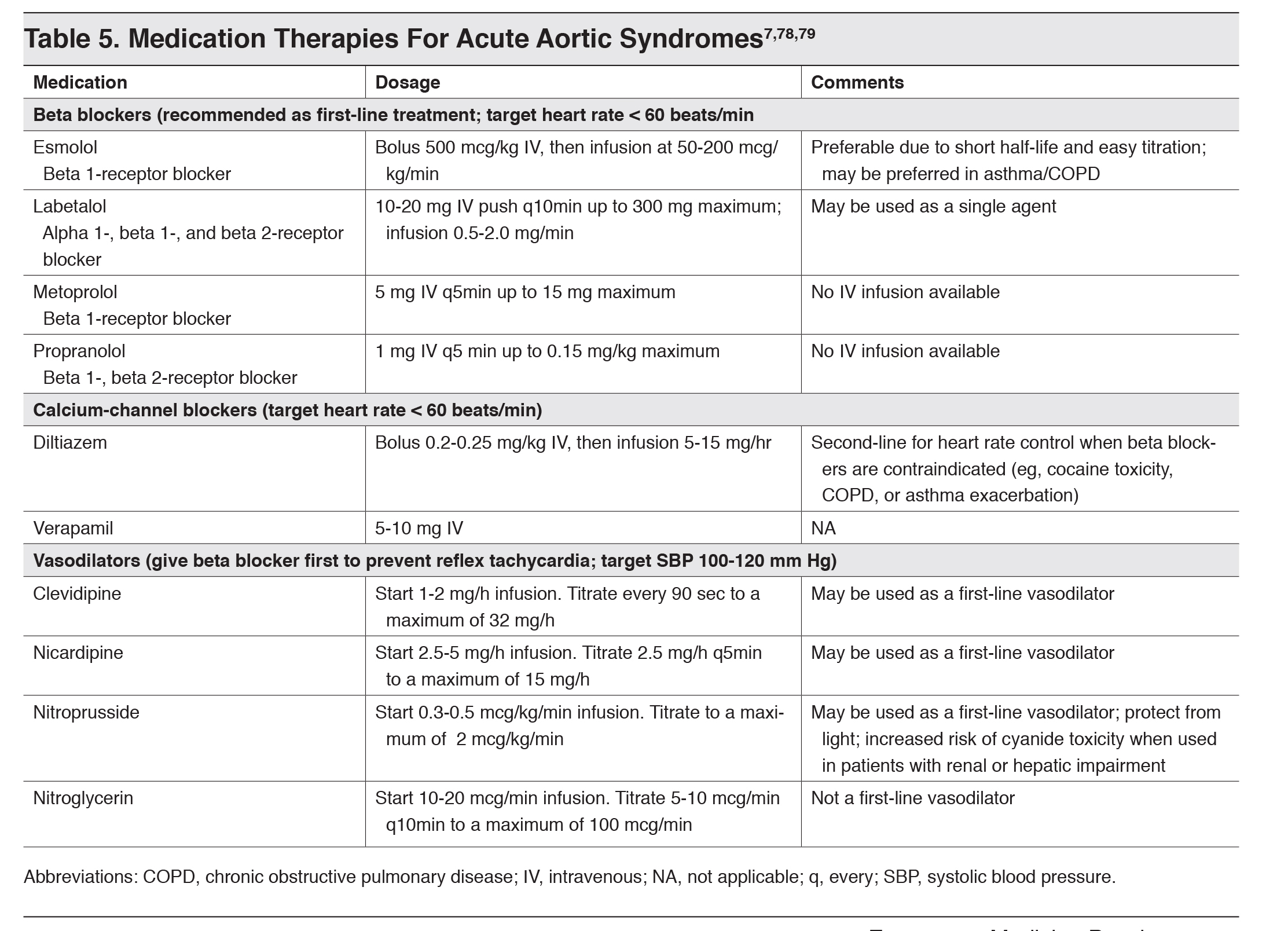
The treatment for aortic dissection is discussed elsewhere, but medical treatment relies on reducing shear forces through the reduction of heart rate to <60 bpm and systolic blood pressure to 100-120. This is achieved via IV beta blockers (first line) or IV dihydropyridine calcium channel blockers (second line), followed by vasodilators. Aggressive pain control with IV narcotics and reversal of anticoagulation should also be considered. Definitive treatment is open surgical vs. endovascular repair.
References
- Davis DP, Grossman K, Kiggins DC, Vilke GM, Chan TC. The inadvertent administration of anticoagulants to ED patients ultimately diagnosed with thoracic aortic dissection. Am J Emerg Med. 2005;23(4):439-42. PMID 16032607.
- Diercks DB, Promes SB, Schuur JD, et al. Clinical policy: critical issues in the evaluation and management of adult patients with suspected acute nontraumatic thoracic aortic dissection. Ann Emerg Med. 2015;65(1):32-42.e12. PMID 25529153.
- Hagan PG, Nienaber CA, Isselbacher EM, et al. The International Registry of Acute Aortic Dissection (IRAD): new insights into an old disease. JAMA. 2000;283(7):897-903. PMID 10685714.
- Hansson EC, Dellborg M, Lepore V, Jeppsson A. Prevalence, indications and appropriateness of antiplatelet therapy in patients operated for acute aortic dissection: associations with bleeding complications and mortality. Heart. 2013;99(2):116-21. PMID 23048167.
- Hirata K, Wake M, Kyushima M, et al. Electrocardiographic changes in patients with type A acute aortic dissection. Incidence, patterns and underlying mechanisms in 159 cases. J Cardiol. 2010;56(2):147-53. PMID 20434885.
- Klompas M. Does this patient have an acute thoracic aortic dissection?. JAMA. 2002;287(17):2262-72. PMID 11980527.
- Leitman IM, Suzuki K, Wengrofsky AJ, et al. Early recognition of acute thoracic aortic dissection and aneurysm. World J Emerg Surg. 2013;8(1):47. PMID PMC3874654.
- Lo BM. An evidence-based approach to acute aortic syndromes. Emergency Medicine Practice. 2013; 15(12). PDF.
- Luo JL, Wu CK, Lin YH, et al. Type A aortic dissection manifesting as acute myocardial infarction: still a lesson to learn. Acta Cardiol. 2009;64(4):499-504. PMID 19725443.
- Ohle R, Um J, Anjum O, et al. High risk clinical features for acute aortic dissection: A case control study. Acad Emerg Med. 2017; epub ahead of print. PMID 29218798



great case. presenting systolic bp is 109. Still giving labetalol?