The Case
CC
R flank pain x 3days
HPI
32 yo M w/no PMH reports 3 days of constant, dull, non-radiating progressively worsening R flank pain. He went to outside hospital 2 days ago and was told that he had kidney stones. Per his CT report he had “minimal R perinephric infiltrative changes without evidence of nephrolithiasis.” He denies a history of previous stones, denies fever, chills, chest pain, shortness of breath, dysuria, hematuria, abdominal or groin pain, illicit substance use, family history of kidney stones/clotting disorders.
Physical Exam
Afebrile, HR 88, BP 155/90, RR 18, SpO2 99% RA
Gen: well-appearing, well-nourished male in NAD
Resp: CTA b/l
CV: RRR, nml S1/2, no m/r/g, 2+ radial/DP pulses
Abd: Soft, +BS, NTP, no m/r/g
Back: R flank tenderness, mild R CVAT
Ext: WWP, no edema
Labs
UA: bland
BMP: 135/4.2/101/30/11/1.013.1/37.2<190
LFTs: 31/51/61/0.6/0.2/6.7/4.0
INR 1.18
PTT 30.5
Lactate 0.6
Media
Questions
-
Describe the CT findings.
There are multiple wedge shaped renal infarcts seen on the R kidney on the two slices. Otherwise, no pathology was noted on the two slices. The rest of the abdomen CT was unremarkable.
-
What is your differential diagnosis?
The most likely cause of multiple wedge-shaped renal infarcts is from thrombi or emboli. The possible etiologies are numerous and include atrial fibrillation, endocarditis, renal artery dissection, aortic dissection, left ventricular thrombus, suprarenal aortic atheroma, fibromuscular dysplasia, Ehlers-Danlos syndrome with thrombotic aneurysm, or a hypercoagulable state (i.e. anti-phospholipid syndrome, vasculitis) or cocaine abuse.
-
What is the appropriate next step in managing this patient?
- EKG to evaluate for atrial arrhythmias
- Echocardiogram to evaluate for atrial or ventricular thrombi
- Additional laboratory testing for HBV, HCV, hypercoagulation panel for evaluating for entities such as antiphospholipid syndrome
- Anticoagulation
- possible long-term blood pressure medication, preferred agents are ACEi or ARB
More Info
Our patient:
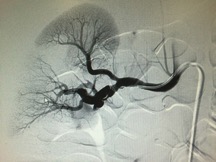
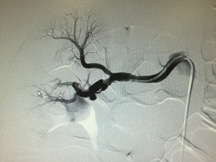
This patient had an unremarkable EKG and was admitted to medicine on a heparin drip for additional evaluation and treatment. The TTE was unrevealing. The patient had an extensive work-up that was largely negative, including thrombophilia panel, HIV, RPR, HBV and HCV. The patient ultimately underwent MRA of kidneys, aorta as well as abdominal arteriogram. The right renal arteriogram (included) “shows irregularity and beading of main trunk together with thrombosis of main renal vessels to lower pole of the kidney and two branches of the upper pole.”
This “beading” and “irregularity” of the renal artery seen on the MRA is consistent with a disease entity known as Fibromuscular Dysplasia (FMD).
FMD is a non-atherosclerotic, non-inflammatory disease in which collagen is deposited abnormally or “dysplastically” in the “fibrous” and “muscular” layers of various major arteries throughout the body. It is this abnormal collagen deposition that ultimately leads to arterial stenosis, dissection, and/or aneurysm, that can affect any arterial bed. Like the patient above, 75-80% of patients have renal artery involvement. Many patients often multiple arteries affected at the same time including the Internal carotid and vertebral, which are also quite common. Disease states affecting the visceral and external iliac arteries can be found, but less commonly affected.
The etiology of FMD is unknown, but possibly due to genetic or hormonal influences. As a result, FMD is much more common in females and found at all ages with medial age of diagnosis of 50s. The female predominance, however, disappears in children. FMD is a radiological diagnosis with the classic “string of beads” or “circumferential or tubular stenosis” appearance. The most common presenting signs and symptoms of FMD patients are hypertension (due to renal artery stenosis), headache, pulsatile tinnitus, neck pain, or cervical bruit (due to abnormalities of the carotid or vertebro-basilar system). Other common complaints are flank or abdominal pain, abdominal bruit, or TIA/CVA. Suspect FMD in patients with above presentations without the usual risk factors such as age >60 years old, coronary artery disease, or hypertension.
Treatment modalities vary on the arterial bed involved and associated symptoms as well as the predicted clinical course. In some cases, medical therapy with anticoagulation and surveillance is reasonable. However, surgical intervention is also common. For arterial stenosis or dissection that require intervention, surgery or angioplasty with or without stenting are often utilized while aneurysm can be corrected with coils and stents.
Our patient was continued anticoagulation in the hospital and was eventually discharged from the hospital on Coumadin with follow-up scheduled with an outside specialist.
Bibliography
- Varennes, L., et al. Fibromuscular dysplasia: what the radiologist should know: a pictorial review. Insights Imaging (2015) 6:295–307.
- Slovet, D. Fibromuscular Dysplasia. NEJM (2004) 350:1862-71.
- Olin, J. Clinical manifestations and diagnosis of fibromuscular dysplasia. In: uptodate.com 2015 August, UpToDate, Waltham, MA. (Accessed 20 September 2015).